Introduction
Total joint arthroplasty, particularly total hip arthroplasty (THA), has become one of the most successful surgical interventions for improving pain, function, and quality of life in patients with end-stage osteoarthritis or post-traumatic joint degeneration.1 As the global population ages and the indications for arthroplasty continue to expand, the annual volume of primary hip and knee replacements has grown substantially.2 According to national registry data, more than 1 million primary THAs are performed annually worldwide, with continued growth projected in both high-income and developing countries.3
However, this success has been accompanied by a parallel increase in postoperative complications. Among these, periprosthetic femoral fractures (PFFs) represent a particularly complex and costly challenge. These injuries can occur intraoperatively or postoperatively and are most often seen in elderly patients with osteoporotic bone and long-standing implants.4 Their management is often surgically demanding, requiring a balance between fracture fixation and prosthetic stability.5 Reported incidence rates of PFF following THA vary from 0.1% to 5%, depending on patient population, implant type, and duration of follow-up.6 In particular, the Vancouver classification system has become the gold standard for stratifying fracture types and guiding treatment algorithms.7
In high-income countries, modular revision stems and advanced locking plates are widely used to manage these fractures.8 However, access to such technology remains limited in many low- and middle-income countries (LMICs), including Central Asia.9 Kazakhstan, like other countries undergoing rapid healthcare modernization, faces challenges in providing cost-effective and reproducible solutions for complex orthopedic injuries.10 In this context, the development and clinical implementation of locally manufactured implants play a crucial role in improving surgical outcomes and accessibility.11
The National Scientific Center of Traumatology and Orthopedics (NSCTO) in Astana is the country’s leading referral institution for complex musculoskeletal trauma and joint reconstruction. As a tertiary-level national center, it receives and manages over 90% of all documented cases of periprosthetic femoral fractures in Kazakhstan. This makes it a representative setting for evaluating both surgical practices and epidemiological patterns related to periprosthetic complications in the region. In recent years, the center has adopted a domestically developed anatomically contoured locking plate system for the management of PFFs, offering a cost-efficient alternative tailored to local anatomical and resource conditions.
Despite the increasing use of this implant, there is a lack of published data evaluating its real-world effectiveness, safety, and clinical applicability. To address this gap, the present study aimed to retrospectively assess the demographic characteristics, fracture types, surgical methods, and early postoperative outcomes of patients with PFFs treated using the national plate system over a five-year period. By analyzing a consecutive series of cases from the NSCTO, we aim to provide evidence supporting the practical value of localized implant strategies in the treatment of complex periprosthetic fractures.
Materials and Methods
This retrospective observational study was conducted at the National Scientific Center of Traumatology and Orthopedics named after Academician N.D. Batpenov (NSCTO) in Astana, Kazakhstan. The study covered a five-year period from January 2020 to December 2024 and included all adult patients who were admitted with a diagnosis of periprosthetic femoral fracture (PFF) following total hip arthroplasty (THA).
All cases were identified through the hospital’s electronic database and confirmed via radiographic imaging. The inclusion and exclusion criteria are summarized in the table.
Each case was assessed for demographic characteristics (age, sex), clinical parameters (ICU stay, duration of hospitalization), and operative details. Fractures were classified according to the Vancouver classification and assigned ICD-10 codes: S72.3 (shaft), S72.4 (distal femur), T84.4 (implant-related complications), and T02.7 (multiple lower limb fractures).
All patients were treated with a locally developed, anatomically contoured locking plate system designed specifically for the femoral morphology in the presence of a prosthetic stem. The plate’s geometry included fixed-angle screw paths in the proximal segment, enabling bicortical fixation around the stem, and additional transverse slots for secure placement of cerclage wires at various diaphyseal levels. All operations were performed using a standard lateral approach under general or spinal anesthesia, with intraoperative fluoroscopic guidance for reduction and implant placement. Perioperative care followed institutional protocols, including antibiotic prophylaxis and thromboembolism prevention.
The primary outcome was defined as the clinical condition at discharge (improved, unchanged, or worsened). Secondary outcomes included ICU admission, postoperative complications, and duration of hospital stay. Data were analyzed using SPSS v27. Descriptive statistics (mean, standard deviation, percentages) were calculated. Welch’s t-test was used for continuous variables with unequal variances, and Pearson’s chi-square test or Fisher’s exact test was used for categorical data. Correlations between age, ICU need, and hospitalization length were analyzed using Spearman’s rank correlation. Statistical significance was set at p < 0.05.
This study received approval from the local ethics committee at NSCTO. Given its retrospective nature and full anonymization of patient data, informed consent was waived according to institutional and national ethical guidelines.
Results
A total of 38 patients who met the inclusion criteria were treated for periprosthetic femoral fractures (PFFs) following total hip arthroplasty (THA) at the National Scientific Center of Traumatology and Orthopedics between 2020 and 2024. All patients underwent surgical treatment using a locally manufactured anatomically contoured locking plate. The cohort demonstrated consistent demographic trends, anatomical fracture patterns, and favorable early clinical outcomes.
Patient Demographics and Epidemiology
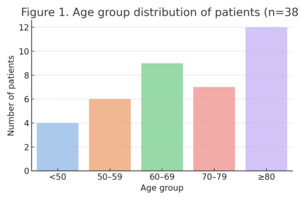
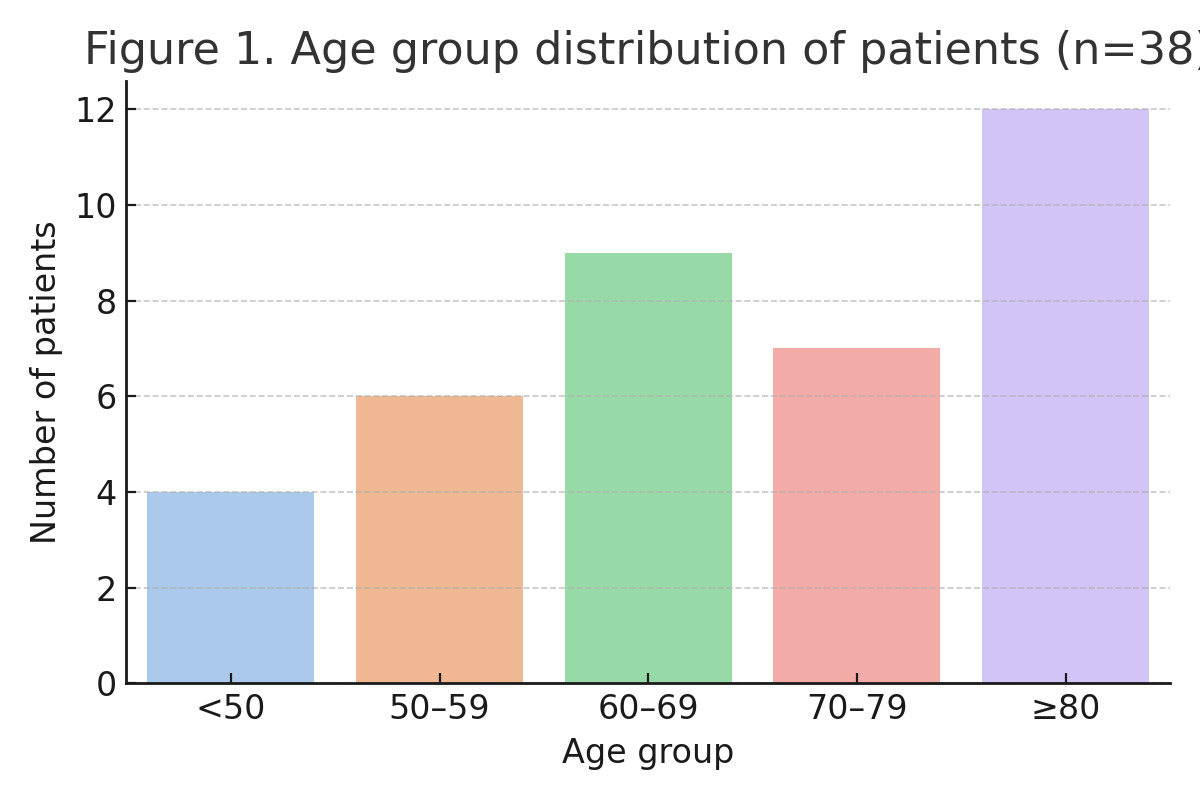
The mean age across the entire cohort was 63.6 years (range: 31–86), with a median of 66. Approximately 39.5% of patients (15 out of 38) were aged 70 years or older. The proportion of elderly patients was highest in 2022 (60%) and lowest in 2021 (22.2%). Females represented the majority of the cohort (63.2%), consistent with established epidemiologic trends in periprosthetic fractures and osteoporotic injury risk. Annual demographic data are presented in Table 1.
Notably, the sex distribution reversed in 2024, with male patients comprising 60% of that year’s cases. Age distribution showed a clustering in the 60–79 age range, but 12 cases (31.6%) involved patients ≥80 years, emphasizing the high-risk profile of the cohort.
Fracture Classification and Mechanism
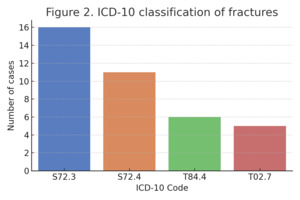
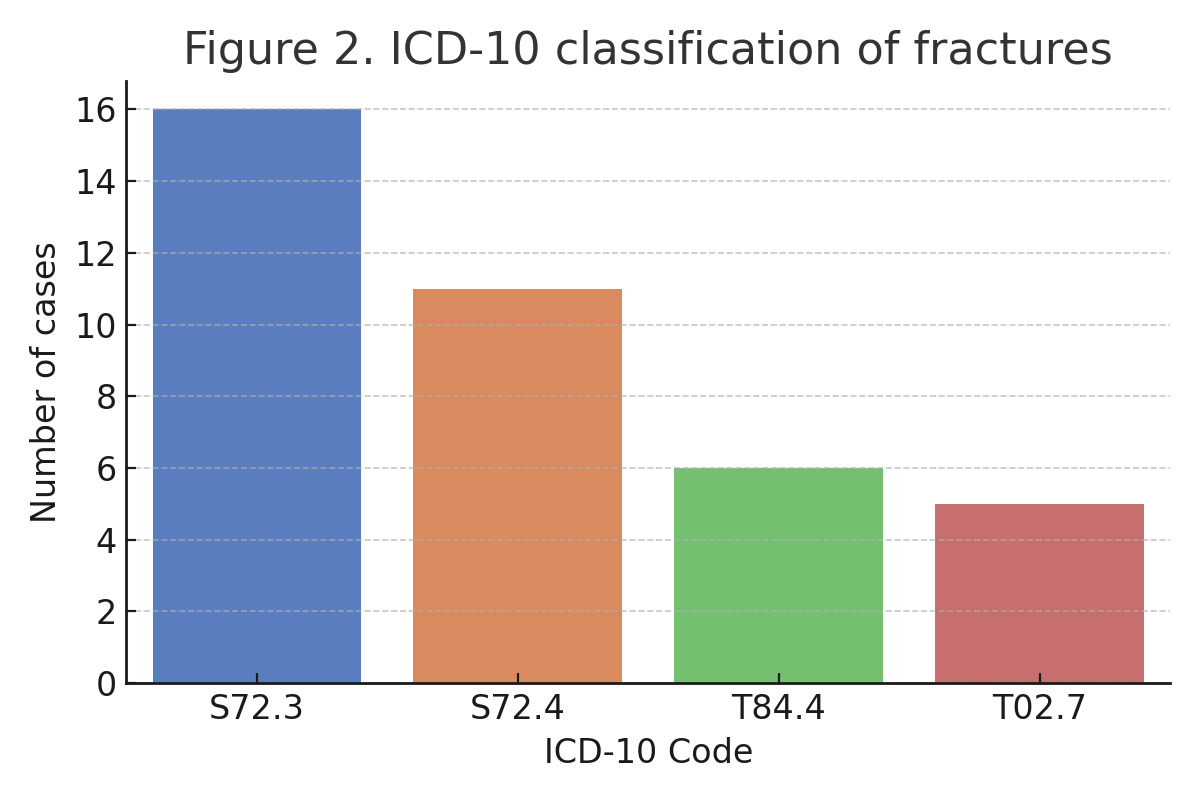
Fractures were categorized radiographically according to ICD-10 codes and Vancouver classification. The most frequent diagnosis was fracture of the femoral shaft (S72.3), accounting for 42.1% of cases, followed by distal femoral fractures (S72.4, 28.9%). A smaller subset involved mechanical complications of the implant (T84.4, 15.8%) and combined lower limb trauma (T02.7, 13.2%).
The majority of fractures occurred as a result of low-energy trauma, primarily ground-level falls. There were no cases of high-energy trauma (e.g., motor vehicle collisions) or intraoperative fractures.
The anatomical distribution is visualized in Figure 2, with a clear predominance of shaft and metaphyseal fractures.
Surgical Management
All patients underwent open reduction and internal fixation with the national locking plate system. The implant’s proximal design facilitated bicortical screw placement despite the presence of a femoral prosthesis. In 73.7% of cases, cerclage wires were used in addition to plate fixation to augment construct stability, particularly in patients with complex comminution or osteoporotic bone. No stem revision procedures were required in any case.
Intensive Care Unit Utilization
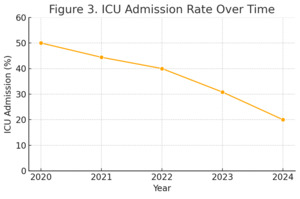
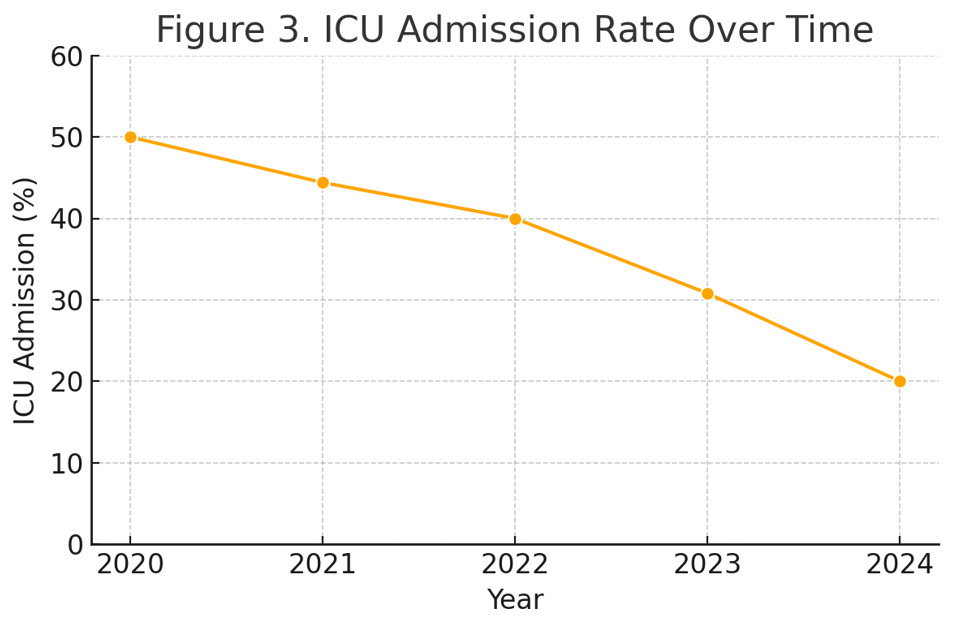
Fourteen patients (36.8%) required admission to the intensive care unit (ICU) during their hospitalization. The rate of ICU admission declined progressively from 50% in 2020 to 20% in 2024, potentially reflecting improvements in perioperative management and early mobilization strategies. Median ICU stay was 2 days (range: 1–7 days). There was no statistically significant association between ICU admission and patient age (p = 0.12), although older age trended toward higher ICU use.
Hospitalization and Clinical Outcomes
Length of hospital stay ranged from 4 to 69 days, with a mean of 21.8 ± 10.4 days. The longest admissions were observed in patients aged ≥75 and those requiring cerclage augmentation. No patient died during the index hospitalization. There were no reported cases of wound infection, dehiscence, reoperation, or hardware failure.
All patients were discharged in improved clinical condition. Discharge destination was home in 89.5% of cases; the remaining patients were referred to regional rehabilitation facilities. No transfers to ICU from regular wards were required postoperatively.
Subgroup and Correlation Analysis
To evaluate the impact of age on clinical outcomes, patients were stratified into two groups: those younger than 70 years and those aged 70 years or older. Patients in the older group had a significantly longer mean hospital stay (27.4 vs 18.3 days; p = 0.045). Although the proportion of ICU admissions was higher among patients aged ≥70 (46.7% vs 30.4%), this difference did not reach statistical significance (p = 0.18). Similarly, the use of cerclage wiring was more frequent in the older group (80.0% vs 69.6%), but the difference was not statistically significant (p = 0.41). Importantly, all patients in both age groups showed clinical improvement at the time of discharge. Correlation analysis using Spearman’s coefficient revealed a moderate positive association between age and length of hospitalization (ρ = 0.39, p = 0.017). A summary of these comparisons is presented in Table 2.
Discussion
Principal Findings and Interpretation
This study provides an institution-level evaluation of periprosthetic femoral fractures (PFFs) treated at Kazakhstan’s national orthopedic referral center over a five-year period. The key findings include: a high prevalence of elderly and female patients; a predominance of femoral shaft and distal femur fractures; no in-hospital mortality; and favorable early outcomes with the use of a domestically developed anatomical locking plate.
The demographic profile in our cohort—mean age 63.6 years, 63.2% female—is consistent with registry data from the UK, Sweden, and Canada, which show that women aged >70 account for the majority of PFF cases.12–14 Our ICD-based classification confirmed that Vancouver type B fractures (S72.3/S72.4) remain the most common, reflecting mechanical stress concentrations at the bone–stem interface, especially in osteoporotic patients. The absence of intraoperative fractures or high-energy trauma cases supports the hypothesis that implant-related fatigue and bone remodeling are key contributors in this population.
Comparison with Published Literature
The outcomes achieved in this series—specifically, the absence of early complications and complete avoidance of stem revision—compare favorably with international benchmarks. Platzer et al. reported a 4.5% in-hospital mortality and 18% complication rate among patients with Vancouver B fractures treated with revision stems.15 Our zero-complication rate may be partially attributable to the surgical technique and implant design, but also reflects the centralized care model employed at our institution.
In terms of ICU utilization, our study documented a notable decline in admissions from 50% to 20% over five years. This aligns with recent trends observed in Enhanced Recovery After Surgery (ERAS) protocols, which emphasize early mobilization, multimodal pain control, and preoperative risk stratification.16 Importantly, our findings show that improved perioperative protocols can be implemented in LMIC settings with measurable benefit.
Impact of Implant Design
The anatomical locking plate used in this study was developed locally at NSCTO to address the specific challenges of PFF fixation in the presence of a well-fixed femoral stem. Several design features merit emphasis:
- The proximal curvature closely mirrors the anatomy of the proximal femur, enabling better surface contact and load distribution
- Fixed-angle screw trajectories in the proximal segment allow for bicortical fixation, bypassing the intramedullary stem without jeopardizing stability
- Multiple transverse cerclage slots reduce the risk of wire migration and permit consistent fracture compression along the shaft
These features likely contributed to the absence of mechanical failure or malalignment in our cohort. In contrast, imported plates designed for broader markets may not adequately address the unique anatomical and resource-based constraints found in Kazakhstan and similar regions.17
Health System Considerations
The National Scientific Center of Traumatology and Orthopedics (NSCTO) functions as a central referral unit for complex orthopedic trauma across Kazakhstan, managing more than 90% of documented PFF cases nationwide. This centralized care model offers an advantage in accumulating surgical expertise, standardizing protocols, and enabling the development and refinement of domestic implant systems.
From a policy perspective, the success of the national plate system demonstrates the value of investing in local implant production. Not only does this reduce dependence on costly imports, but it also facilitates rapid iterations based on clinical feedback. In the context of LMICs, where budgetary and logistical barriers often hinder adoption of Western devices, domestically tailored solutions offer a pragmatic pathway to improving surgical equity.18
Figure Reference
A representative case is presented in Figure 4, showing both the preoperative and postoperative radiographs. The anatomic placement of the plate, proper screw angulation, and supplementary cerclage demonstrate the principles outlined above and the real-world applicability of this technique in high-risk patients.
Strengths and Limitations
This study is one of the first to report outcomes from a nationally representative cohort in Central Asia treated with a domestic implant system. The centralized data source, uniform surgical team, and five-year observation period strengthen internal consistency and clinical applicability. However, several limitations must be acknowledged.
Limitations
First, the retrospective design restricts causal inferences and is vulnerable to documentation bias. Second, while the NSCTO captures the majority of national cases, the single-center nature of the study may limit generalizability to smaller regional hospitals. Third, long-term outcomes such as functional status, implant survivorship, and radiographic healing were not evaluated. Finally, the sample size (n=38) remains modest despite the duration of data collection. These limitations underscore the need for future multicenter prospective trials with functional follow-up.
Conclusion
Periprosthetic femoral fractures represent an increasingly significant clinical and economic burden, particularly in aging populations undergoing total hip arthroplasty. The findings of this five-year institutional study demonstrate that a domestically produced anatomically contoured locking plate can provide reliable fixation and favorable short-term outcomes without the need for stem revision or modular revision systems. The absence of early complications, combined with consistent clinical improvement, highlights the safety and effectiveness of this implant strategy in the treatment of complex periprosthetic fractures.
Importantly, this study underscores the feasibility of deploying locally manufactured, anatomically adapted implants in low- and middle-income countries, where access to imported solutions remains limited. The centralized surgical model at the National Scientific Center of Traumatology and Orthopedics, which manages the majority of such cases in Kazakhstan, offers a replicable framework for scalable, cost-effective orthopedic care.
These findings support the integration of context-specific implant systems into national surgical protocols and validate the role of centralized expertise in achieving high-quality outcomes. Future multicenter prospective studies with long-term follow-up and functional assessment are essential to confirm the durability of these results and guide implant development for broader international application.
Conflict of Interest
The authors declare that they have no competing interests.
Funding
This research was funded by the Science Committee of the Ministry of Science and Higher Education of the Republic of Kazakhstan (Grant No. BR21881815-OT-24).
Ethics Approval and Consent to Participate
The study protocol was approved by the institutional ethics committee of the National Scientific Center of Traumatology and Orthopedics (NSCTO), Astana, Kazakhstan. Given the retrospective nature of the analysis and full anonymization of patient data, the requirement for informed consent was waived in accordance with institutional and national guidelines.
Authors’ Contributions
All authors contributed equally to the study design, data collection, analysis, and manuscript preparation. All authors read and approved the final version of the manuscript.
Acknowledgements
The authors would like to thank the surgical and administrative team of the NSCTO for their clinical contributions and logistical support during the study period.
Author Contributions
Balgazarov Amanzhol — Conceptualization, Writing – Original Draft, Methodology, Surgery, Supervision
ORCID: https://orcid.org/0000-0002-4932-0377
Balgazarov Serik — Investigation, Surgery, Data Collection
ORCID: https://orcid.org/0000-0003-4193-7695
Batpen Arman — Methodology, Data Collection, Validation
ORCID: https://orcid.org/0000-0002-6661-8132
Rimashevskiy Denis — Statistical Analysis, Visualization, Writing – Review & Editing
ORCID: https://orcid.org/0000-0001-8122-5815
Abilov Ruslan — Surgery, Resources, Data Curation
ORCID: https://orcid.org/0000-0003-2309-628X
Kriklivyy Alexandr — Data Collection, Radiographic Analysis, Formal Analysis
ORCID: https://orcid.org/0000-0002-5675-047
Atepileva Aliya — Data Curation, Literature Review, Writing – Review & Editing
ORCID: https://orcid.org/0000-0003-4342-8317
Ramazanova Aigul — Writing – Review & Editing, Validation, Ethics Coordination
ORCID: https://orcid.org/0009-0002-9503-2197
Alzhanov Yersultan — Conceptualization, Writing – Review & Editing, Corresponding Author
ORCID: https://orcid.org/0000-0002-6348-9080
Conflict of Interest
The authors declare that they have no competing interests.
Funding
This research was funded by the Science Committee of the Ministry of Science and Higher Education of the Republic of Kazakhstan (Grant No. BR21881815-OT-24).