I. INTRODUCTION
Until now, many authors have discovered varieties of upper limb nerve compression disorders, the most typical being carpal tunnel syndrome caused by median nerve compression at the wrist. Posterior interosseous nerve entrapment is a rare upper limb neuropathy with an incidence of only 0.003%,1 which can be found in patients with or without a history of trauma, due to local compressive components such as a ganglion cyst,2,3 lipoma4 at the elbow, or even with spontaneous hourglass-shaped nerve compression.5 The characteristic of this condition is a gradual paralysis of the finger extension, while the patient’s wrist can still extend. Muscles atrophy may occur if the disease is not treated properly.
We report a clinical case of a male patient with a healthy medical history. Five months before hospitalization, there was a gradual onset of weakness in finger extension. The patient underwent a clinical examination, and an MRI was performed which did not reveal any compressive mass. Electromyography showed posterior interosseous nerve damage in the upper one-third of the forearm, with increased cross-sectional area in the affected segment. The patient was diagnosed with posterior interosseous nerve entrapment, primarily suspected to be due to narrowing at the “supinator tunnel,” and was indicated for nerve release surgery. Four months post-surgery, the patient has partially regained the ability to extend their fingers.
II. CASE REPORT
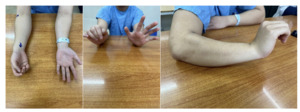
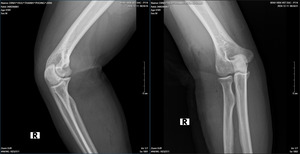
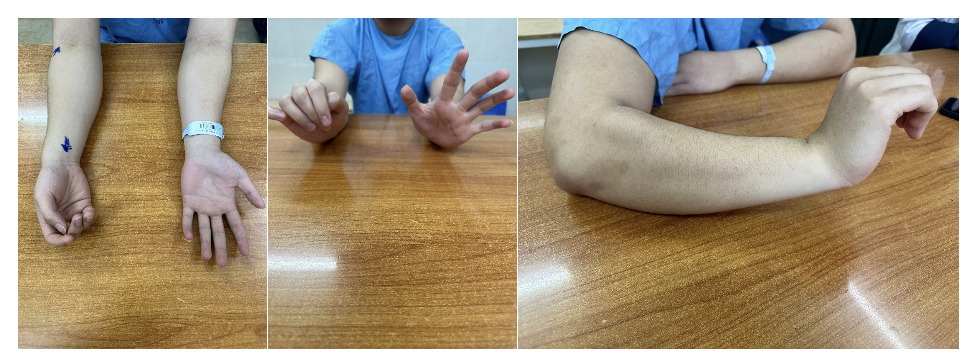
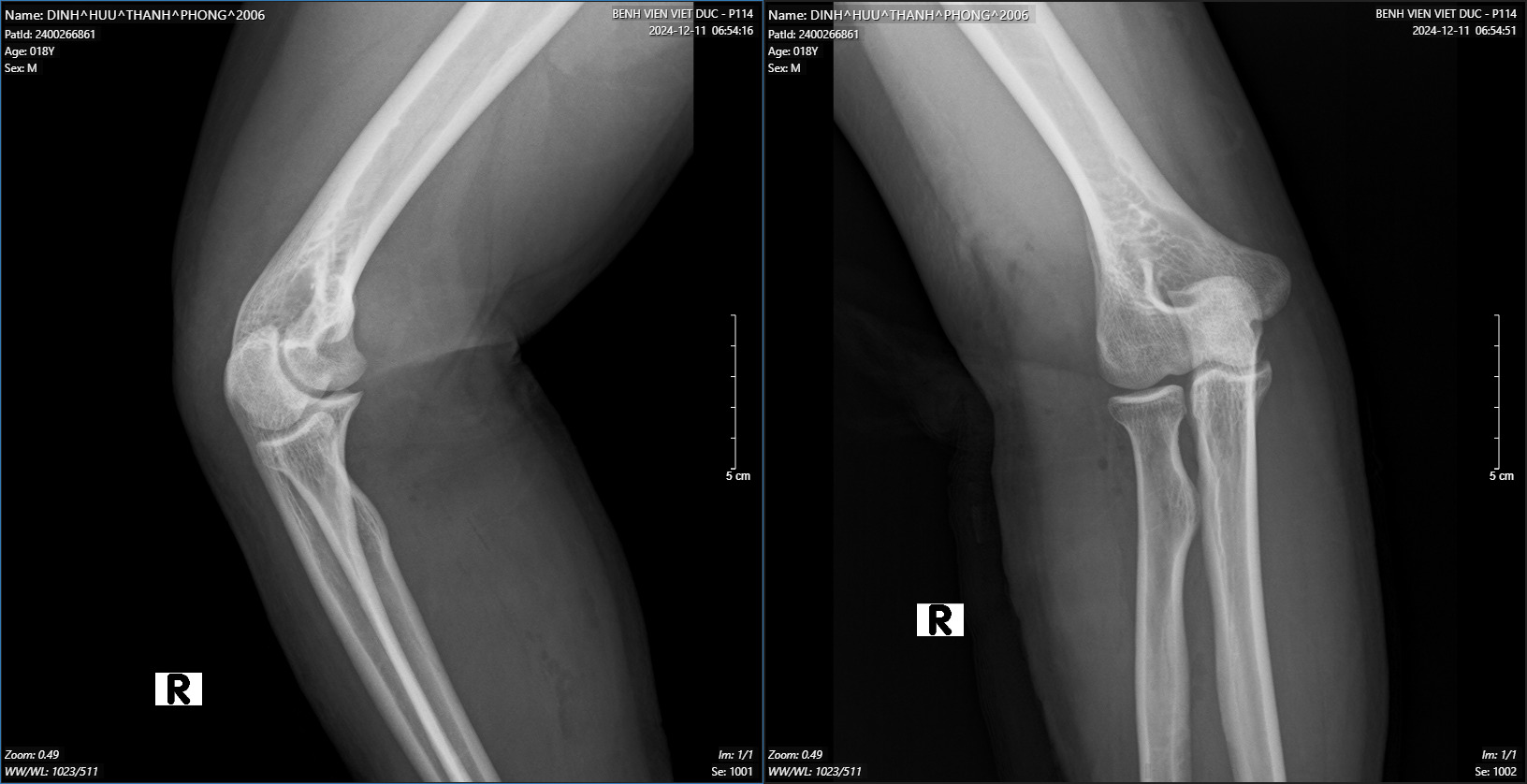
We present a case of an 18-year-old male patient, with a history of healthy development, no previous injuries in the elbow or forearm area. Five months before being admitted to the hospital, the patient began to experience progressively weakness in finger extension. Clinical examination showed the patient had normal shoulder joint movement, normal elbow extension, normal wrist extension, loss of extension and abduction of the thumb, loss of extension of the index, middle, and ring fingers, and weak extension of the little finger. On X-ray of the forearm, no bone lesions were noted, and MRI of the forearm showed no abnormalities. The patient was indicated for an upper limb nerve ultrasound, which showed a posterior interosseous nerve injury over a 25mm segment in the upper third of the forearm near the elbow. The segment of the nerve injury was noted to have an increased diameter, while the segments before and after the nerve injury were of normal size. The patient was diagnosed with posterior interosseous nerve entrapment syndrome and was indicated for nerve decompression surgery. The anterolateral approaching incision was 15 centimeters long, going between the brachioradialis and the extensor carpi radialis longus to access the radial nerve. During the surgery, we found that the patient’s posterior interosseous nerve was compressed by the Leash of Henry in the radial tunnel and primarily by the fibrous band of the supinator muscle at the Arcade of Frohse, where the interosseous nerve passes through the supinator to the posterior lateral side. The posterior interosseous nerve was completely decompressed at five locations, and the patient was discharged after one day with a follow-up appointment and a schedule for regular rehabilitation. After 4 months of surgery, the patient has partially regained the ability to extend their fingers.
III. DISCUSSION
In terms of anatomy, the radial nerve is formed from the C6, 7, 8 branches of the brachial plexus. The nerve travels with the deep brachial artery behind the triceps muscle, and in the lower third, it goes around to the front, piercing through the lateral intermuscular septum. About 10 cm from the lateral epicondyle, the radial nerve branches into motor branches for the brachialis, supinator, extensor carpi radialis longus, and extensor carpi radialis brevis muscles. At this point, the radial nerve passes around the lateral epicondyle, dividing into the superficial branch of the radial nerve that innervates sensation and the posterior interosseous branch. The posterior interosseous nerve, primarily a motor branch, travels in front of the neck of the radius, reaching the Arcade of Frӧhse and entering the posterior forearm through the supinator muscle. Passing through the supinator muscle, the posterior interosseous nerve (PIN) branches off to innervate the extensor carpi ulnaris (ECU), extensor digitorum communis (EDC), extensor digiti quinti (EDQ), abductor pollicis longus (APL), extensor pollicis longus (EPL), extensor pollicis brevis (EPB), and extensor indicis proprius (EIP) in the aforementioned order.6 With the early branching of the radial nerve to the wrist extensor muscles, we can explain why a patient with posterior interosseous nerve compression can still extend their wrist despite losing the ability to extend their fingers.
On examination, we found that our patient had symptoms of low radial nerve palsy: loss of extension and abduction of the thumb, loss of extension of the index, middle, and ring fingers, weak extension of the little finger. Still he had normal wrist extension. To diagnose the patient, we performed routine X-rays of the forearm, forearm MRI, electromyography, and peripheral nerve ultrasound. Imaging tests help identify the cause of nerve compression, which then guides the treatment approach. Many authors worldwide have reported discovering nerve compression masses through direct examination and supported MRI imaging. Fitzgerald4 et al reported 5 cases of lipomas in the forearm compressing nerves, including 4 cases compressing the posterior interosseous nerve and 1 case of a large lipoma compressing both the superficial branch and the PIN of the radial nerve. Maldonado7 et al also reported 2 clinical cases of lipomas directly compressing the posterior interosseous nerve, one lipoma located at the proximal border of the supinator muscle, and the other at the distal border of the supinator muscle. Park3 reported another cause of posterior interosseous nerve compression being a ganglion cyst. The X-ray results of our patient showed no bone lesions, and the MRI also did not reveal the presence of a space-occupying mass. On the other hand, the results of the electromyography indicate a complete posterior interosseous nerve injury, and the nerve ultrasound shows a localized nerve injury segment of 25mm in the upper third of the forearm near the elbow, with a slight increase in the size of the injury segment, while the segments before and after the injury are of normal size. Based on the clinical and paraclinical examination information, we are leaning towards posterior interosseous nerve entrapment syndrome, primarily caused by compression at the “radial tunnel.”
The anatomy of the “Radial Tunnel” was first described in 1954 by two authors, Michelle and Krueger,8 and is defined as a tunnel approximately 5cm long from the elbow to the proximal border of the supinator muscle, surrounded by anatomical landmarks. The brachioradialis muscle mostly forms the upper wall and part of the lateral wall along with the extensor carpi radialis brevis muscle. The floor of the tunnel is the radius bone and the proximal border of the supinator muscle.9 In this radial tunnel, there are 5 common sites where the radial nerve and posterior interosseous nerve can be compressed, including: the fibrous band between the biceps brachii and brachioradialis muscles in front of the elbow joint, the recurrent ulnar artery, also known as Leash of Henry, the medial border of the extensor carpi radialis brevis muscle, the proximal border of the supinator belly, also known as Arcade of Frӧhse - first described in 1908 by the same author Frӧhse, and the distal border of the supinator. The Arcade of Frӧhse is where the posterior interosseous nerve passes through the supinator muscle to go to the lateral side, and it is also the most common site of compression of the posterior interosseous nerve.10
With the patient’s paralysis symptoms gradually worsening, the patient was indicated for posterior interosseous nerve release surgery. Reviewing medical literature worldwide, there are many surgical approaches to access the posterior interosseous nerve, such as the anterior forearm approach between the BR and brachialis muscles or through the BR muscle, the anterolateral approach between the BR and ECRL muscles, and the posterior approach between the EDC and the ECRB muscles. Urch11 et al studied the above surgical approaches and concluded that the anterior and anterolateral approaches provide access to 4/5 of the most commonly compressed positions of the posterior interosseous nerve, while the posterior approach offers the clearest view of the distal border of the supinator muscle. We chose the anterolateral approach extending between the BR and the ECRL, with the anatomical feature of the posterior interosseous nerve running from front to back through the supinator. The surgical approach was a 15cm incision on the upper one-third of the anterior lateral forearm, dissecting between the BR and the ECRL to directly expose the posterior interosseous nerve. During the surgery, we found that the patient’s PIN, after branching from the radial nerve, was primarily compressed at two locations: one at the Leash of Henry and the other at the supinator muscle at the Arcade of Frӧhse. The anterior segment compressing the posterior interosseous nerve was enlarged, increasing in diameter, while the surrounding blood vessels nourishing the nerve sheath remained intact. We cut the vessels of the Leash of Henry, releasing the entire posterior interosseous nerve at all 5 positions up to the distal border of the supinator muscle.
The patient was discharged at one day post-op and was scheduled for regular follow-up and rehabilitation sessions. At the follow-up examination 4 months post-op, the patient was quite satisfied with the surgery as he had regained partial extension function from the second to the fifth finger; however, the first finger still could not extend or abduct. It is necessary to continue monitoring and rehabilitation exercises for the patient.
IV. CONCLUSION
Posterior interosseous nerve entrapment is a rare upper limb neurological condition with a very low incidence. The typical clinical feature of the disease is a gradual paralysis of finger extension without losing wrist extension. The disease is diagnosed through clinical and paraclinical examinations. MRI and electromyography are particularly important for diagnosing the cause of compression as well as differentiating it from other conditions. In cases where the cause of compression is at the radial tunnel, the posterior interosseous nerve needs to be decompressed at all five most commonly compressed sites. The results of the surgery after 4 months have helped the patient partially regain the ability to extend their fingers, but further long-term monitoring is still needed.


__exposing_the_pin_(1)_being_compressed_by_the_leash_of_henr.png)



__exposing_the_pin_(1)_being_compressed_by_the_leash_of_henr.png)

