INTRODUCTION
Hallux varus is a relatively rare but functionally disabling deformity, characterized by medial deviation of the great toe at the level of the first metatarsophalangeal (MTP) joint.1 While congenital, post-traumatic, or systemic causes are recognized,2–4 the most common etiology in adults is iatrogenic — a complication arising from surgical overcorrection of hallux valgus deformities.5–7 Reported incidence rates of iatrogenic hallux varus vary from 2% to 17%, depending on the surgical technique and intraoperative handling of soft tissues.5,7–9
The pathophysiology of iatrogenic hallux varus involves an imbalance between medial and lateral stabilizers of the first MTP joint. Over release of lateral structures, excessive medial capsulorrhaphy, or aggressive bone resection can lead to progressive varus deviation, often accompanied by pain, instability, difficulty with footwear, and cosmetic dissatisfaction.4,5 If untreated, the deformity may progress to rigid clawing of the hallux, degenerative joint changes, and significant impairment of gait.1,5,6
Numerous surgical techniques have been described to address this condition, including tendon transfers, capsular balancing procedures, and first MTP joint arthrodesis.4,5,9–12 While arthrodesis remains a reliable option for rigid deformities with joint degeneration,6,13 it sacrifices mobility. In contrast, soft tissue reconstructive techniques aim to preserve joint function, particularly in cases without significant arthritic changes.5
However, the optimal surgical approach for flexible, non-arthritic iatrogenic hallux varus remains debated. Techniques based on local soft tissue rearrangement may offer a less invasive and joint-preserving alternative, yet evidence regarding their efficacy is limited.5 In this study, we use the term myoligamentoplasty to describe a soft tissue–based surgical technique that reconstructs the medial stabilizers of the first metatarsophalangeal (MTP) joint using autologous capsular and ligamentous structures, occasionally supported by adjacent musculotendinous tissues. This method is intended to restore alignment and function without resorting to tendon transfers or arthrodesis.
The objective of this study was to evaluate the mid-term clinical and radiographic outcomes of local soft tissue myoligamentoplasty in patients with iatrogenic hallux varus following failed hallux valgus surgery. By presenting a single-center case series, we aim to contribute additional data to the existing body of knowledge and assess the viability of this technique as a function-preserving surgical option.
METHODS
Study Design and Setting
This was a retrospective, observational case series conducted at the Department of Orthopedic Surgery, a tertiary-level referral center specializing in foot and ankle pathology. The study period spanned from January 2022 to January 2025. Ethical approval was obtained from the institutional review board (Protocol 6), and all patients provided written informed consent prior to inclusion.
The study adhered to the principles of the Declaration of Helsinki and followed the STROBE guidelines for reporting observational studies.
Patient Selection
Patients were eligible for inclusion if they met all of the following criteria:
-
Age ≥ 18 years;
-
History of hallux valgus correction surgery resulting in clinically and radiographically confirmed iatrogenic hallux varus (IHV);
-
Persistent symptoms of pain, functional limitation, or dissatisfaction with foot appearance;
-
Absence of degenerative changes in the first metatarsophalangeal (MTP) joint on weight-bearing radiographs;
-
Availability of complete clinical and radiographic data at baseline and at 12-month follow-up.
Exclusion criteria were:
-
Congenital, traumatic, or neuromuscular forms of hallux varus;
-
Rigid deformities with severe joint arthrosis (Grade III or higher according to Coughlin’s classification);
-
Previous revision surgeries for hallux varus;
-
Inflammatory joint disease or systemic neuromuscular conditions (e.g., rheumatoid arthritis, Charcot-Marie-Tooth disease);
-
Loss to follow-up or refusal to participate.
A total of seven female patients (seven feet) fulfilled the inclusion criteria and were enrolled. The mean age at the time of revision surgery was 61.5 ± 5.9 years (range: 46–63 years). All patients had previously undergone modified McBride procedure for hallux valgus correction.
The mean interval between the primary hallux valgus surgery and the revision procedure for IHV was 2.3 ± 1.1 years. No bilateral interventions were performed.
Surgical Technique
All procedures were performed by the same senior orthopedic surgeon under spinal anesthesia with sedation. Patients were placed in the supine position with a pneumatic tourniquet applied to the mid-thigh. A strict sterile protocol was followed throughout the procedure.
Step 1: Medial Approach and Capsular Flap Preparation
An arcuate medial incision was made along the line of the previous scar, extending from the distal one-third of the first metatarsal shaft to the proximal phalanx. Dissection was carried down through the subcutaneous tissue and medial capsule. A tongue-shaped capsular flap was created, based proximally at the base of the proximal phalanx. The first MTP joint was exposed, and a careful medial capsular release was performed to mobilize the great toe and correct the varus deviation.
Step 2: Flap Elongation and Lateral Transfer
The capsular flap was reshaped into an “F” configuration, ensuring enough length for lateral transfer. A second longitudinal dorsal incision (~3 cm) was made in the first intermetatarsal space over the previous scar line. Fibrotic and scar tissue between the first and second metatarsals was excised to reduce tension and facilitate graft positioning.
Step 3: Fixation of the Graft
The prepared flap was transferred laterally and sutured to the lateral base of the proximal phalanx of the hallux and the inferolateral aspect of the capsule of the second MTP joint. Non-absorbable braided sutures (e.g., 2-0 Ethibond) were used for fixation in a tension-free, anatomically corrected position. The toe was held in neutral alignment and gently dorsiflexed to assess the stability of correction.
Step 4: Closure
Layered wound closure was performed with absorbable sutures for deep tissue and nylon sutures for skin. A bulky sterile dressing was applied with gentle compression. No Kirschner wires or implants were used.
Postoperative Management
Postoperative care followed a standardized rehabilitation protocol. The hallux was immobilized in a neutral position using a toe splint. Starting from the second postoperative day, patients were allowed partial weight-bearing using a rigid-soled postoperative shoe (such as Barouk) designed to offload the forefoot. Skin sutures were removed on day 12. Patients continued wearing orthopedic shoes for the following 4–5 weeks, after which they gradually transitioned to soft, comfortable footwear for an additional 7–8 weeks. Return to regular footwear and full weight-bearing was typically permitted approximately 12 weeks after surgery.
Rehabilitation Protocol
A standardized rehabilitation protocol was initiated in the second postoperative week. It included passive and active range of motion exercises targeting the first metatarsophalangeal (MTP) joint to restore mobility. Patients also performed strengthening exercises aimed at reactivating the intrinsic muscles of the foot. Gait training was conducted under the supervision of a physiotherapist to ensure proper walking mechanics. Additionally, physiotherapy modalities such as low-intensity pulsed magnetic therapy were used to reduce soft tissue swelling and promote tissue healing.
Outcome Measures
Clinical and radiographic assessments were performed at baseline (pre-op), 3 months, and 12 months postoperatively.
Clinical Assessment
Clinical assessment included evaluation of pain severity using the Visual Analog Scale (VAS), where 0 represented no pain and 10 indicated the worst pain imaginable. Functional outcomes were measured using the American Orthopaedic Foot and Ankle Society (AOFAS) Hallux-MTP-IP score, with a maximum of 100 points. Subjective satisfaction was also documented and categorized as “completely satisfied,” “satisfied with minor concerns,” or “satisfied with major reservations.”
Radiographic Assessment
Radiographic assessment was based on standardized weight-bearing anteroposterior (AP) foot radiographs obtained at all evaluation time points. Two angular parameters were measured: the intermetatarsal angle (IMA), defined as the angle between the first and second metatarsals, and the hallux valgus angle (HVA), defined as the angle between the first metatarsal and the proximal phalanx of the hallux. All measurements were independently performed by two orthopedic surgeons who were blinded to the clinical outcomes. To minimize interobserver variability, the final values were calculated as the average of the two readings.
Statistical Analysis
All statistical analyses were performed using Microsoft Excel 2021 and Jamovi v2.3 (open-source statistical software). Continuous variables are reported as means ± standard deviations (SD) and ranges. To evaluate the significance of changes in clinical and radiographic outcomes between preoperative and postoperative assessments (3 and 12 months), the Wilcoxon signed-rank test for paired samples was applied. This non-parametric test was chosen due to the small sample size (n=7) and the potential for non-normal distribution of the data.
The following variables were compared using the Wilcoxon test:
-
Visual Analog Scale (VAS) pain scores;
-
AOFAS Hallux-MTP-IP scores;
-
Intermetatarsal angle (IMA);
-
Hallux valgus angle (HVA).
A p-value < 0.05 was considered statistically significant.
RESULTS
A total of seven female patients (seven feet) with symptomatic iatrogenic hallux varus were included in the study. All patients had previously undergone hallux valgus correction using the modified McBride technique. The mean age at the time of revision surgery was 61.5 ± 5.9 years (range, 46–63), and the average time from primary to revision procedure was 2.3 ± 1.1 years. All cases were unilateral (right: 4, left: 3). No intraoperative complications or postoperative reoperations were recorded. Detailed demographic and surgical characteristics are summarized in Table 1.
Clinical Outcomes
All patients experienced a notable reduction in pain and improvement in foot function at 12 months postoperatively. The mean Visual Analog Scale (VAS) score for pain decreased from 6.5 ± 0.7 preoperatively to 1.2 ± 0.2 at final follow-up, indicating significant symptomatic relief (p = .0156). Functional assessment using the AOFAS Hallux-MTP-IP score improved from a baseline mean of 33.9 ± 6.1 to 78.0 ± 7.0 (p = .0156), reflecting substantial gains in mobility, weight-bearing capacity, and footwear tolerance. No patients reported worsening of symptoms or functional decline. Individual preoperative and postoperative outcome scores are summarized in Table 2. Statistically significant improvements were observed in both VAS and AOFAS scores (p = 0.0156), and the HVA correction was consistent across all cases (p = 0.0156).
Radiographic Outcomes
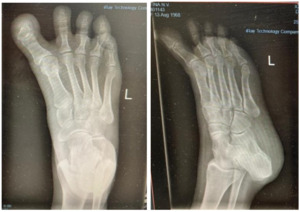
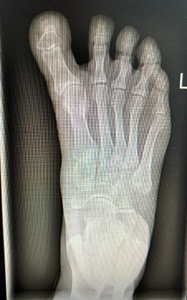
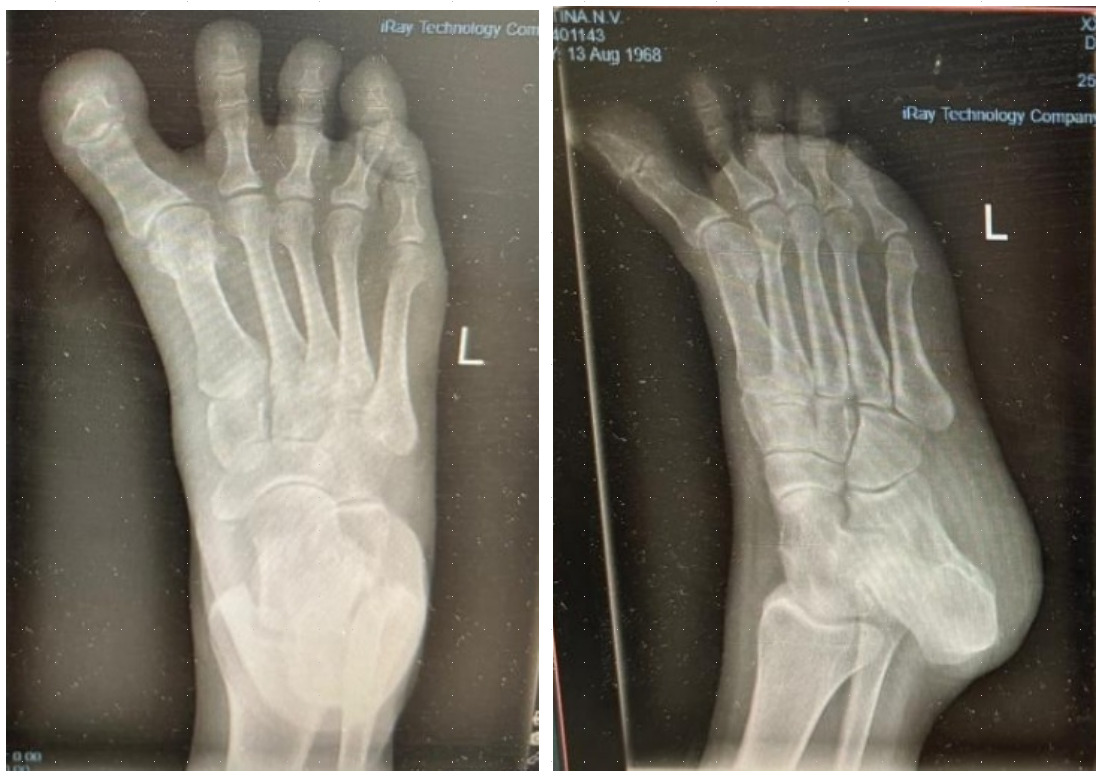
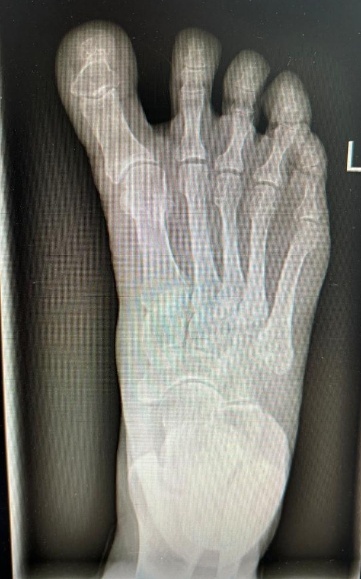
Radiographic evaluation demonstrated effective correction of the hallux alignment. The mean hallux valgus angle (HVA), which was negative in all cases preoperatively (mean –16.5° ± 4.2), improved significantly to a postoperative mean of 5.7° ± 3.2 (p = .0156), with all patients achieving alignment within the physiologic range. Representative radiographs are presented in Figures 1 and 2.
The intermetatarsal angle (IMA) remained stable, changing minimally from a preoperative mean of 3.9° ± 1.6 to 3.7° ± 1.4 postoperatively (p = .6547), suggesting that the procedure achieved targeted realignment of the great toe without affecting the overall first-ray geometry.
Patient Satisfaction
All patients expressed subjective improvement in foot function, pain, and appearance. Five patients rated their outcomes as “completely satisfied,” and two were “satisfied with minor concerns.” No dissatisfaction or requests for additional surgical revision were recorded. Representative pre- and postoperative clinical photographs illustrating cosmetic improvement in toe alignment are shown in Figure 3.
DISCUSSION
Iatrogenic hallux varus remains a complex and functionally limiting complication, particularly when it occurs after soft tissue–based corrections such as the modified McBride procedure. The deformity is often associated with chronic pain, limited mobility of the great toe, footwear difficulties, and dissatisfaction with foot appearance, all of which can significantly impair quality of life.4 Surgical management must carefully balance correction of alignment with preservation of joint function, particularly in cases without degenerative changes. In this context, our study assessed the efficacy of local soft tissue myoligamentoplasty as a revision procedure for flexible hallux varus deformities in patients previously treated for hallux valgus.
Our mid-term outcomes demonstrated substantial improvements in both pain (VAS) and function (AOFAS) across all patients. These clinical benefits were accompanied by statistically significant correction of the hallux valgus angle (HVA), which was maintained throughout the follow-up period, indicating durable structural realignment. Notably, the intermetatarsal angle (IMA) remained stable, suggesting that the procedure achieved targeted medial soft tissue stabilization without compromising the broader forefoot architecture. This mechanical neutrality may be critical in preserving the native biomechanics of the first ray and preventing secondary deformities.
These findings are consistent with prior literature supporting the use of soft tissue reconstruction in flexible or semi-rigid hallux varus. Leemrijse et al.14 reported favorable results using reverse abductor hallucis tendon transfer, with consistent pain relief and functional gains. Similarly, Maynou et al.9 achieved good outcomes in 11 of 12 cases through tendon transfer techniques tailored to deformity severity. While effective, these techniques typically require harvesting of additional structures, which introduces donor site morbidity and can prolong operative time. In contrast, our method relies entirely on local capsular and ligamentous tissues, thus avoiding the need for tendon grafts.
Fuhrmann15 described functional recovery following extensor hallucis longus (EHL) tendon transfer but also noted complications such as residual stiffness and discomfort during ambulation. These were not encountered in our series, possibly due to the joint-sparing and minimally invasive nature of the myoligamentoplasty technique. Moreover, our patients experienced improved MTP joint mobility and gait stability, emphasizing the value of preserving dynamic function in cases without arthrosis.
In cases of rigid deformity or degenerative changes, arthrodesis remains the standard of care. Belfiore et al.,6 in a decade-long series, demonstrated reliable correction and symptom relief with first MTP joint fusion in such patients. However, fusion inevitably sacrifices joint motion and may not be well-tolerated by relatively younger or active patients. In our cohort, the absence of joint space narrowing or osteoarthritic changes enabled the use of a joint-preserving procedure. This distinction underscores the importance of careful preoperative selection, as myoligamentoplasty is best suited for flexible deformities with preserved cartilage.
In addition to clinical effectiveness, our technique offers several surgical advantages. It is technically reproducible, requires no specialized instrumentation, and can be performed through familiar medial and dorsal approaches. The use of an F-shaped capsular flap allows for precise control of tension and alignment, which can be adjusted intraoperatively based on the degree of residual deformity. Furthermore, the double-incision technique facilitates scar excision and avoids lateral soft tissue tethering — a known cause of recurrence in previous procedures.
Although mild residual varus alignment was noted in a few cases, no patient experienced clinical recurrence, progression of deformity, or the need for reoperation during the follow-up period. This observation suggests that minor undercorrection may, in fact, be biomechanically favorable by maintaining soft tissue balance and minimizing the risk of overcorrection into valgus. This principle may be especially relevant in elderly patients, in whom functional improvement and pain relief often outweigh the need for complete radiographic normalization.
Lastly, the economic and logistical advantages of this approach should not be underestimated. Unlike tendon transfer or implant-based techniques such as suture-button constructs (e.g., Mini TightRope),9 myoligamentoplasty is cost-effective, as it avoids synthetic materials, allografts, or specialized implants. The procedure relies solely on native autologous tissues and standard surgical instruments, making it particularly attractive in resource-limited healthcare systems. In light of growing emphasis on sustainable, high-value care, biologically simple and reproducible techniques such as this offer meaningful advantages in terms of cost, accessibility, and long-term safety.
Taken together, our results reinforce the role of local soft tissue myoligamentoplasty as a viable, joint-sparing surgical option for correcting flexible iatrogenic hallux varus. The technique is effective, safe, reproducible, and minimally invasive, providing favorable clinical and radiographic outcomes without sacrificing joint motion or requiring extensive reconstruction. Its strategic use in properly selected patients may expand the treatment paradigm for this challenging deformity.
Limitations
Despite the favorable outcomes observed in this series, several limitations warrant consideration. First, the study included a small number of patients (n = 7), limiting statistical power and generalizability. However, iatrogenic hallux varus is an uncommon condition, and similar studies in the literature often rely on small cohorts due to its rarity. In this context, even limited series can contribute meaningful clinical insights, particularly when supported by consistent methodology and detailed outcome reporting.
Second, the retrospective nature of the study introduces inherent risks of selection and observer bias. While objective outcome measures and standardized follow-up protocols were employed, including independent radiographic assessment by blinded reviewers, prospective validation is necessary to minimize these biases.
Third, the follow-up period of 12 months allows only for mid-term evaluation. Although no recurrences or complications were observed during this time, longer-term monitoring is essential to determine the durability of correction, potential joint degeneration, or delayed complications, particularly in active or younger patients.
Finally, the absence of a control group limits the ability to directly compare this technique with other established revision strategies, such as tendon transfers or MTP arthrodesis. Future comparative studies will be required to better define the relative advantages and limitations of myoligamentoplasty within the broader treatment algorithm.
Future Directions
Building on the positive mid-term results of this study, future investigations should aim to validate the technique through prospective, multicenter trials with larger patient populations. Standardization of surgical technique, rehabilitation protocols, and outcome assessment tools—including patient-reported outcome measures (PROMs)—will be critical to improving reproducibility and cross-study comparisons.
Additionally, randomized or matched comparative studies evaluating myoligamentoplasty against tendon transfer procedures, suture-button constructs, or arthrodesis would help delineate the optimal indications for each technique. Biomechanical analysis of soft tissue tensioning and capsular remodeling over time could provide further insight into the physiological basis of long-term stability.
Longitudinal follow-up extending beyond two years would be especially valuable for identifying delayed recurrences, radiographic progression of joint changes, and the impact of residual deformity on gait mechanics and quality of life.
CONCLUSION
This case series highlights the potential of local soft tissue myoligamentoplasty as a safe, effective, and motion-preserving surgical solution for flexible iatrogenic hallux varus in patients without significant degenerative changes. The technique achieved consistent clinical and radiographic improvements, with no observed complications or need for reoperation during mid-term follow-up.
Its reliance on autologous tissues, avoidance of synthetic implants, and minimal morbidity profile make it a particularly attractive option in both high-resource and resource-constrained settings. Moreover, the joint-sparing nature of the procedure preserves first MTP mobility—an important advantage in active individuals or those seeking to avoid fusion.
While further research is needed to confirm its long-term efficacy and to compare it with other revision strategies, our findings support the inclusion of myoligamentoplasty as a viable and reproducible component of the surgical armamentarium for managing this complex and infrequent deformity.

_and_12-month_postoperative_(right)_clinical_photographs_showing_correc.png)
_and_12-month_postoperative_(right)_clinical_photographs_showing_correc.png)