Introduction
Tibial shaft fractures are the most common long bone fracture accounting for 16.9 to 22 cases per 100,000 people annually and are observed in 4% of the adult population.1,2 The OTA/AO classification is most commonly used in research and considers the location of the fracture, energy, and mechanism required to cause fracture.3 Larsen et al. reported AO classification 42-A1 as being the most common tibial shaft fracture type, representing 34% of all fractures; the study also reported females represented 36.2% of patients studied with most fractures occurring during low-energy trauma while males represented 63.8% of patients with most fractures occurring during high-energy trauma and sports injuries.1 Low-energy tibial shaft fractures typically occur from torsional force resulting in spiral fractures. High-energy mechanisms are usually from direct trauma, can cause wedge or short oblique fractures of the tibial shaft with significant comminution, and can be associated with soft tissue injury, compartment syndrome, bone loss, and ipsilateral skeletal injury.4,5 Treatment options for tibial shaft fractures in skeletally mature individuals include cast immobilization, open reduction and internal fixation with plates and screws, external fixators, and intramedullary nailing (IMN). While treatment options for tibial shaft fractures vary based on factors including open injury, severity of fracture, and soft tissue status, IMN has emerged as the preferred definitive option for stabilization in adults.6–8 IMN of the tibia in flexion has been traditionally utilized to achieve reduction and fixation of proximal third tibial shaft fractures.9 The tibial approaches for IMN placement include suprapatellar and infrapatellar entry points. Utilization of the optimal entry point for each patient and fracture pattern is paramount for minimizing soft tissue injury, intraarticular exposure, malalignment of the fracture, and knee pain.10,11 Therefore, the primary purposes of this review and cadaveric study are to evaluate entry points for reamed tibial nails for tibial shaft fractures and the risks, benefits, and advantages of each technique.
Background
The healing outcome of a long bone fracture is determined by the mechanical environment when the blood supply is adequate.12 The gap size, stiffness of the construct, and interfragmentary motion are determined by quality of reduction, fixation system stability, and functional loading; this process influences the type (endochondral versus primary) and rate of bone healing.12 After success of reamed IMN in the femur, reamed IMN of unstable tibia fractures became more popular.13 Reamed IMN has become the mainstay of treatment for most adult tibial shaft fractures due to minimal soft tissue dissection, good bone union rate, and early return to daily living.14 Cast immobilization is appropriate for low-energy tibial fractures with minimal soft tissue dissection; however, fractures with higher energy mechanisms involving more osseous and soft tissue disruption make closed reduction difficult to obtain and maintain.13,15 In a study of 201 tibial shaft fracture cases, Puno et al. reported IMN resulted in lower complication rates with one nonunion (1.7%), two infections (3.3%), and no malunions in 60 patients compared to closed reduction and casting, which resulted in 14 delayed unions or nonunions (9.9%), two infections (1.4%), and six malunions (4.3%) in 141 patients.16 Alho et al. also demonstrated functional results being superior with IMN than bracing in a series of 78 patients with displaced tibial shaft fractures (35 with bracing and 43 with IMN).15 Traditional plate fixation is not as commonly used as it requires extensive soft tissue dissection potentially further devitalizing the bone, and it is not a load-sharing construct.13 In a randomized clinical trial examining disability ratings at 6 and 12 months after distal tibia fracture treatment, Costa et al. documented patients with IMN fixation had less disability earlier in their rehabilitation, better ankle function, and improved health-related quality of life at 3 and 6 months when compared to traditional locking plate fixation.17
Complications of Tibia Fractures
Tibial shaft fractures have been frequently associated with a myriad of complications. Acute complications following injury include compartment syndrome, nerve damage, vascular injury, and infection especially in the setting of high energy and open fractures.18,19 Anterior knee pain is the most common patient complaint after IMN with a variable incidence ranging from 28.6% to 65%.20–23 The etiology of knee pain following tibial nailing is multi-factorial and may still occur after using any of the approaches for IMN.24 Subsequent surgery following tibial IMN placement has often been noted in up to 18% of all patients with painful hardware cited as the most common cause.25 Other reasons for reoperation include malunion and nonunion.
The advent of IMN has largely reduced the incidence of angular malunion and limb shortening in patients with improved anatomic alignment, however rotational malalignment has remained a concern.26 In order to minimize malrotation, new strategies such as the use of external tibial aiming devices during IMN placement have demonstrated a significant reduction in malrotation.27 Although malunions occur in 8-10% of all tibial shaft fractures, the incidence has been reported as high as 50% in proximal-third tibial shaft fractures with valgus and procurvatum deformities being most common.16,28,29
Nonunions have a multifactorial etiology and can result from patient-related factors and/or non-modifiable risk factors. Patient-related factors for tibial shaft nonunions include smoking, obesity, diabetes, alcohol use, and impaired nutritional status. Fong et al. determined tibial shaft fractures with <25% cortical continuity had the highest predictive value for nonunion and reoperation with the presence of a fracture gap, open fractures, and transverse fractures also contributing to a high risk of nonunion.30,31 Several treatment options exist for nonunions including exchange nailing, bone grafting, and nail dynamization.32–34 When a septic nonunion is present, eradication of infection is necessary prior to management via a staged approach.35,36
With technological advancements, different approaches and positioning techniques have been developed to mitigate complications, aid in fracture reduction, and avoid joint perforation.22,37,38 These include the infrapatellar approach to the tibia, which consists of patellar tendon splitting (transpatellar) versus patellar tendon sparing (medial and lateral parapatellar) and the suprapatellar approach. The newer lateral parapatellar semi-extended approach has also gained popularity and warranted further study.
Suprapatellar
The suprapatellar approach for IMN of the tibia allows for easier patient and injured leg positioning while also mitigating deforming forces on the fracture to aid reduction during nail placement.39 Suprapatellar nailing utilizes standard AP and lateral fluoroscopy views along with a more direct pathway for nail placement, and it has been reported to help minimize malalignment and malunion associated with proximal tibia fractures.40,41 By relieving quadriceps tension, the typical apex anterior angulation of the proximal fragment is minimized, resulting in improved fracture reduction while also protecting the patellar tendon.42,43 This approach theoretically protects both the patellar tendon and the infrapatellar nerve, and patients may experience less postoperative anterior knee pain during flexion.44,45 Sanders et al. performed a study of 37 patients treated with suprapatellar nailing of the tibia and reported the absence of anterior knee pain in all 37 subjects at their one-year follow-up.46 Macdonald et al. examined the differences in anterior knee pain by comparing the suprapatellar and infrapatellar approaches for tibial IMN using the Aberdeen Weightbearing Test – Knee (AWT-K) and demonstrated a greater proportion of weight transmitted through the injured leg than uninjured leg in the suprapatellar group versus the infrapatellar group signifying more weight was tolerated and less pain was experienced in the suprapatellar group.47 While the risk to intraarticular structures such as the articular cartilage of the patella and trochlea is a concern with the suprapatellar approach, a cadaveric study by Gaines et al. compared the suprapatellar approach with the standard medial parapatellar entry and noted a lower rate of intra-articular injuries when using the suprapatellar approach.48 Additionally, surgeons can avoid or minimize soft tissue damage in open tibial fractures with this approach due to the increased distance between optimal incision point and potential area of soft tissue injury.43 The suprapatellar approach is, however, intraarticular such that the knee joint itself is exposed to the local environment during nailing, and there are concerns of causing intra-articular injury and infecting the knee joint.39 If there is potential for gross contamination or known infection in the tibia during nailing or exchange nailing for infected nonunions, this approach could seed infection to the knee joint itself.
Infrapatellar
The traditional infrapatellar approach for tibia IMN involves placing the knee in hyperflexion before inserting the nail through a transpatellar or parapatellar technique.49 To avoid damage to intraarticular structures and achieve excellent fracture reduction, the “ideal” entry point for insertion of a tibial nail has been described as being 2 mm medial to the lateral tibial spine on AP imaging and immediately adjacent and anterior to the articular margin of the medial tibial plateau on lateral imaging.50 Anderson et al. performed a study comparing entry point and nail insertion accuracy between infrapatellar IMN and suprapatellar IMN techniques demonstrating the mean entry point of an infrapatellar IMN as 1.3mm anterior and 2.9mm medial to the ideal entry point, and the mean entry point of a suprapatellar IMN as 3.5mm anterior and 3.4mm medial to the ideal entry point.50,51 However, as the mean entry point for the infrapatellar group was closer to the “ideal” starting point in both coronal and sagittal planes, it was also reported to contain greater variance and thus inferior nail insertion accuracy as compared to the suprapatellar technique.50
Infrapatellar nailing has also been commonly associated with anterior knee pain with reported incidence varying from 10 to 80%.49 Sun et al. performed a comparison study between infrapatellar and suprapatellar techniques demonstrating the VAS pain score as being significantly lower in the suprapatellar group than the infrapatellar group at 6, 12, and 24 months.22,23,49,52 Additionally, Yang et al. performed a meta-analysis of 4 randomized control trials and reported IMN with the suprapatellar approach compared to the infrapatellar approach was associated with not only a significant reduction in total blood loss, VAS scores, and fluoroscopy times, but also a significant improvement in Lysholm knee scores.44 Conversely, Chan et al. documented no significant difference in VAS scores between an infrapatellar approach and suprapatellar approach after 12 months (1.5 and 0.36, respectively).53
Transpatellar
In the transpatellar technique, an incision is made over the patellar tendon and the tendon is split longitudinally with its fibers over the length of the tendon. The transpatellar tendon approach provides direct access to center of the tibia and avoids malpositioning of the nail due to pressure of the tendon against the guide, reamers, and nail itself.54 However, splitting the patellar tendon may be associated with a higher incidence of knee pain due to incision through the tendon and retro-tendinous fat pad which is highly innervated.55,56 Sadeghpour et al. demonstrated the medial parapatellar approach to have a significantly less pain with lower VAS scores at 3 and 6 months when compared to the transpatellar approach for IMN of the tibia; however, Rijal et al.reported no significant difference when comparing these two approaches at 2, 4, and 12 weeks.57,58 Fracture patterns that require extension of the knee can be challenging with use of the transpatellar approach as the patella can engage the insertion handle for the nail limiting the ability to fully extend to the necessary degree to achieve a reductions in certain fracture patterns.
Medial Parapatellar
In the medial parapatellar tendon approach, an incision is made along the medial border of the patellar tendon. The medial parapatellar approach for IMN of the tibia is helpful in reducing the deforming forces, allowing reduction of proximal fractures, and preventing a procurvatum deformity; however, this approach as well as the lateral parapatellar approach requires larger incisions for nail insertion versus the transpatellar approach.57 Medial parapatellar approaches have also been demonstrated to have an increased risk of valgus malunion in proximal tibia fractures.48 Ahmad et al. compared Visual Analog Scores (VAS) between medial parapatellar tendon approach and the transpatellar tendon approach demonstrating that anterior knee pain is significantly less with a medial parapatellar tendon approach than a transpatellar tendon approach (2.5 versus 4.4, respectively) if other causes of anterior knee pain are avoided such as a prominent nail and damage to intra-articular structures during reaming.55 This finding is consistent with Sadeghpour et al. who documented a significant increase in mean anterior knee pain score via VAS after 3 months with the transpatellar approach in comparison to the medial parapatellar approach (2.2 versus 0.72, respectively).57
Lateral Parapatellar
As an alternative to traditional infrapatellar tibial nailing originally described by Küntscher in the 1940s, Tornetta first reported the utility of the intraoperative semi-extended position (15-20° knee flexion) when reducing and nailing proximal tibial fractures.59,60 Recognizing the intra-articular risk while nailing, Tornetta later documented the safe zone for tibial nail placement to be slightly lateral to the tibial tubercle based on cadaveric dissections.11 Semi-extended nailing was originally proposed to optimize patient positioning, fracture reduction, fluoroscopic assessment, and implant insertion.46,59 Since that time, the suprapatellar and parapatellar approaches have been modified to incorporate the semi-extended position when nailing the tibia. At one-year follow-up, Rothberg et al. demonstrated patients with a fractured tibia who were treated with IMN using an extra-articular semi-extended parapatellar approach did not have increased anterior knee pain compared to uninjured controls.61 In a recent systematic review, Ibrahim et al. reported improved pain and function with semi-extended nailing as compared to traditional infrapatellar nailing.62 With the intent of avoiding intra-articular injury to the knee, Kubiak et al. described a novel technique in 2010 using the semi-extended position while performing an extra-articular lateral parapatellar approach during tibial nail placement.63 The lateral parapatellar approach utilizes an incision made at the inferior pole of the patella just medial to the lateral edge of the patellar tendon and extended distally with retraction of the patellar tendon medially. In a prospective cohort study of 70 patients, Stella et al. noted this extra-articular lateral parapatellar approach in the semi-extended position to be an effective technique with nearly complete recovery of knee function and negligible incidence of anterior knee pain at a minimum follow-up of 24 months.64 Additionally, Sharma et al. compared the lateral parapatellar technique and transpatellar technique demonstrating the lateral parapatellar cohort had less anterior knee pain and had a slightly better knee arc of motion than the transpatellar cohort, and utilization of the lateral parapatellar approach decreased morbidity and facilitated early rehabilitation.56
Despite the potential benefits reported with this technique, concerns about violating the joint capsule and the generalized applicability of this technique to everyday practice persist. With a growing population of patients who have undergone or will undergo total knee arthroplasty, this technique can also be utilized for tibial nailing avoiding intra-capsular penetration. Success with a transpatellar approach for IMN has been demonstrated by Devendra et al. in one case study of 3 patients who sustained tibial shaft fractures distal to the location of total knee arthroplasty prostheses.65 Similarly, Haller et al. documented utilization of an IMN with a transpatellar technique in a fracture of the distal tibia, successfully avoiding the tibial baseplate, providing stable fracture fixation, and allowing for early weight bearing.66
Therefore, the secondary goal of this study was to evaluate whether a lateral intramedullary tibial nail can be routinely placed extra-articularly without compromising the integrity of the joint capsule which would be paramount in patients with an infected or grossly contaminated tibia or with total knee implants present.
Materials and Methods of Cadaveric Study
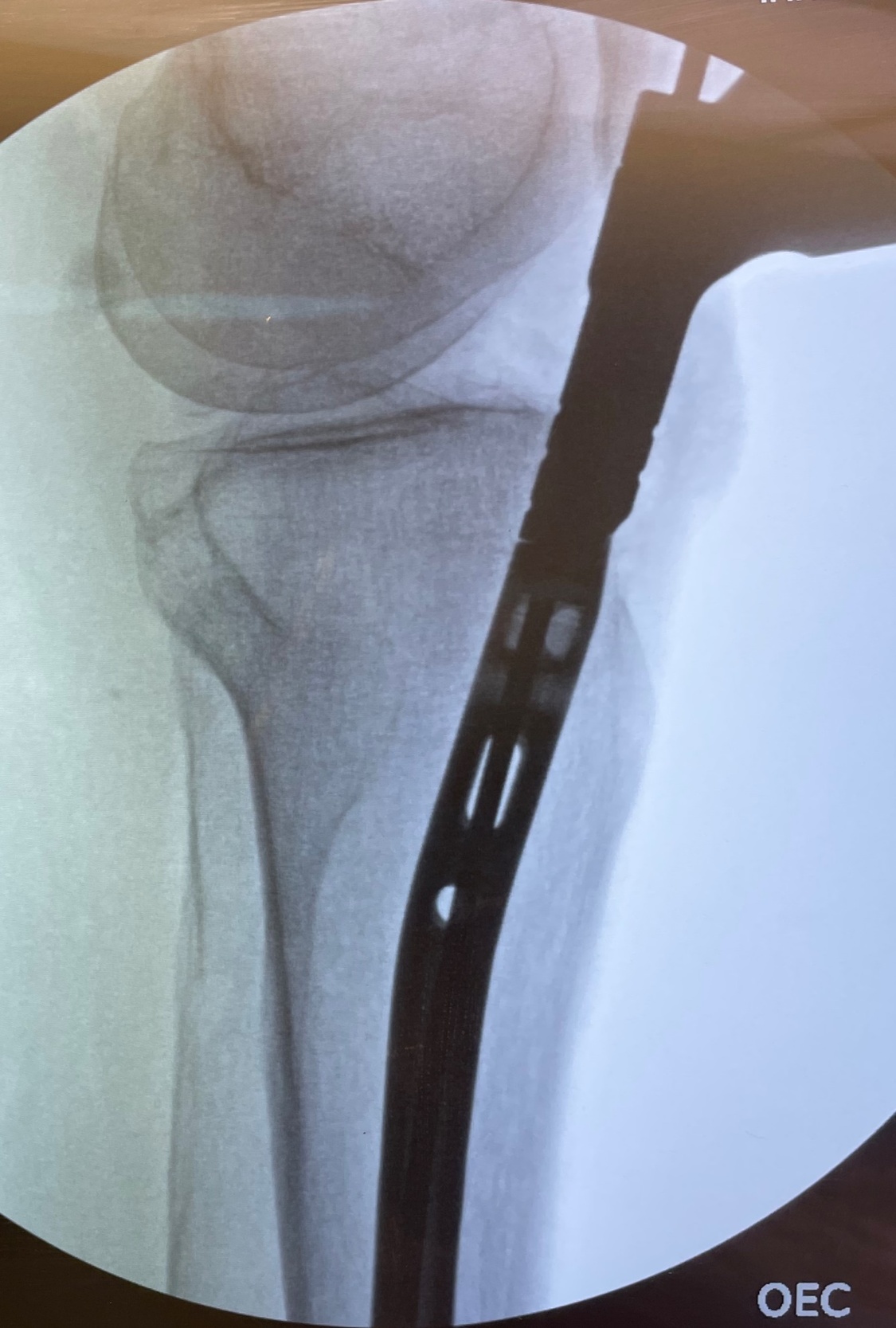
After Institutional Review Board exemption, three paired (6 total) fresh-frozen adult cadaveric lower extremities with intact knee joints were included in the study. With each cadaveric extremity in the semi-extended position, an extra-articular, lateral parapatellar approach was utilized for IMN placement of an unfractured tibia. First, a bump was placed under the ipsilateral hip, then the knee was flexed to 20° and stabilized such that the tibia was parallel to the floor, simulating semi-extended positioning. A lateral parapatellar incision was made through the skin, and meticulous dissection of the retinaculum and surrounding tissue was performed to reveal the proximal tibia per the technique described by Kubiak et al.63 A short Kirschner wire (K-wire) was then inserted deep to the patellar tendon and superficial to the synovium and advanced to the tibial tubercle. The intended entry position was slightly lateral to the center of the tibial tubercle. The K-wire was drilled into the tibia, and fluoroscopic anteroposterior (AP) and lateral imaging of the knee was used to confirm the correct entry position (Figure 1). An opening cannulated reamer was placed over the K-wire to open the canal. The K-wire and reamer were removed, and a long ball-tipped guidewire was inserted and advanced to the most distal aspect of the tibia as confirmed by fluoroscopy. The length of the tibia measured by the guidewire was recorded for nail selection. Next, the intramedullary canal of the tibia was initially reamed with a flexible 9 mm reamer, then in increasing 0.5 mm increments until the appropriate diameter was reached. A Stryker T2 Alpha Nail (Stryker Ltd, Kalamazoo, MI) of appropriate diameter and length was placed into the tibia with fluoroscopic imaging confirming successful positioning (Figure 2).
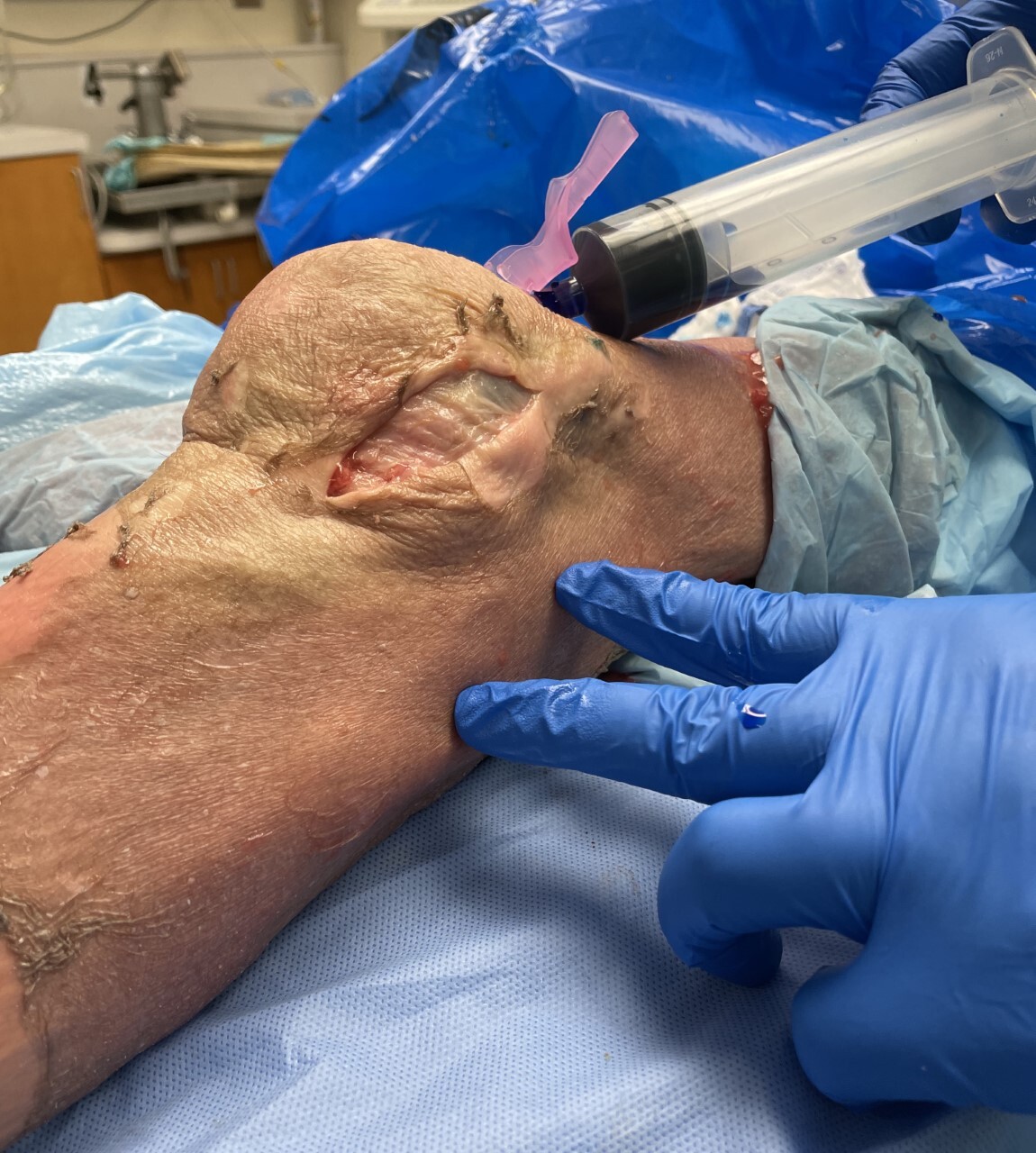
A joint challenge was then performed to assess patency of the knee joint capsule using a superolateral approach. Due to previous literature documenting a 155 cc threshold for joint challenging, a 155 cc mixture of 1% methylene blue and normal saline was injected into the knee joint, and the knee was ranged 15 times to ensure dispersion of the dye.67,68 Lastly, the knee was examined for extravasation of fluid from the lateral incision site. Leakage of methylene blue was interpreted to indicate iatrogenic violation of the joint capsule, and the absence of leakage was presumed to indicate preserved integrity of the joint capsule.
Results
Of the 3 paired cadaveric specimens, 2 were from male donors and 1 was from a female donor. The average age of death of the specimens was 77 years with a range of 66 to 87 years. Three fellowship-trained orthopaedic trauma surgeons with varied experience utilizing extra-articular lateral parapatellar semi-extended tibial nailing participated in the study. Each surgeon performed tibial nailing on both the left and right lower extremities of the same cadaveric specimen. Fluoroscopic imaging confirmed correct entry point lateral to the midline of the tibial plateau. Appropriately sized nails were placed in each cadaver. Placement of tibial intramedullary nails in of all six cadaveric lower extremities was successfully performed utilizing the semi-extended lateral parapatellar approach without violating the integrity of the knee joint capsule. There was no leakage of the methylene blue from any of the six lateral incision sites (Figure 3).
Discussion
The present study demonstrated the semi-extended lateral parapatellar approach to be a reproducible technique regardless of experience with the technique. Each fellowship trained orthopaedic trauma surgeon was able to successfully perform the technique described in Kubiak’s original guide without violating the joint capsule. All orthopaedic surgeons in the current study performed a meticulous dissection to avoid damage to the retinaculum, surrounding tissue, and joint capsule during the surgical approach.
Although retrograde nailing of open femurs has been argued to be a potential conduit for knee sepsis, this risk has been documented to be relatively low at 1.1% by O’Toole et al.69 With similar concerns of having knee sepsis from open tibial fractures, Mitchell et al. noted open tibial shaft fractures treated with an intramedullary nail to have a low risk of knee sepsis despite intra-articular exposure when performed via a suprapatellar approach.70 Furthermore, Tang et al. documented open reduction techniques in the treatment of closed tibial shaft fractures to also have minimal risk of infections.71 Regardless of surgical technique, immediate antibiotic prophylaxis given to patients with open tibia fractures has been reported to improve outcomes by minimizing the risk of deep infections.72 The extra-articular semi-extended lateral parapatellar approach may have the potential to further reduce the risk of knee sepsis in patients with concerns for seeding the knee joint. This may be especially relevant to the post-total knee replacement population to avoid potential prosthetic joint infection.
At an infection rate reported as high as 62.5% following treatment with a reamed intramedullary nail, high-energy open tibia fractures have an increased risk of reoperation, may go on to nonunion, and present a challenge to orthopaedic surgeons despite advancements in treatment options.73–77 While it has been successful by functioning as a biological stimulus, bone grafting for tibial nonunions is limited by segmental defect size, donor site morbidity, and incorporation time.78 Plate osteosynthesis provides another option for management of tibial nonunions as deformity correction can be performed at any location along the diaphysis of the bone. However, patients with compromised skin integrity from open injuries may develop mechanical instability from an infection, which may further inhibit fracture healing.79 Tibial nailing has been an effective method for treating nonunion as mechanical stability is achieved but can also be prone to infection especially if external fixation was initially used to treat an open fracture.80 With all patients healing their open infected tibial nonunions and regaining functionality, Selhi et al. reported antibiotic-impregnated cement nails provide structural support by stabilizing fractures in addition to treating infection at the surgical site.81 Bhatia et al. further demonstrated antibiotic cement impregnated nailing as a single stage procedure to be an effective treatment option for infected tibial nonunions by providing osseous stability and delivering high concentrations of local antibiotics at the infection site without causing systemic toxicity.82 Therefore, the extra-articular semi-extended lateral parapatellar approach may be helpful in minimizing the spread of infection to the joint in cases of open infected tibial nonunions when antibiotic cement impregnated nailing is selected as the treatment option.
There are several limitations to this study. None of the cadaveric specimens in this study had a tibial shaft facture with surrounding soft tissue injury, therefore no reduction maneuvers were performed as would be done in vivo. A small number of specimens were used, which was adequate to demonstrate the success of technique but did not allow comprehensive statistical analysis. To decrease variability, this study only used a nailing system from one manufacturer. While this provided consistency throughout the experiment, different results may be achieved with other manufacturers and designs. Finally, no control specimens were available to test other techniques due to the limited supply of three cadavers. Despite these limitations, the intention of this study was to confirm the extra-articular maintenance and demonstrate the reproducibility of the semi-extended lateral parapatellar approach for tibial nailing.
Conclusion
There are several options for definitive fixation of a tibial shaft fracture, and IMN has emerged as the preferred option for skeletally mature individuals. While the traditional infrapatellar approaches for IMN of the tibia are effective and well documented, the more recently described suprapatellar and semi-extended lateral parapatellar approach are becoming increasingly common as emerging studies have demonstrated reduced post-operative knee pain. It was also confirmed that the semi-extended lateral parapatellar approach can also be successfully performed without compromising the integrity of the joint capsule with varying prior experience with the technique. Knowledge of these approaches as well as their limitations and advantages can aid surgeons in choosing the most appropriate approach for each patient.
Acknowledgement
The authors would like to thank the Rita A. Richardson for her laboratory service and technical expertise.
Author Contributions
A.P.: Cadaver dissection, Literature review, Writing manuscript, Editing manuscript
J.W.: Literature review, Writing manuscript, Editing manuscript
O.L.: Study Design, Cadaver Dissection, Editing manuscript, Final manuscript approval
A.R.: Cadaver dissection, Data collection, Literature Review, Writing Manuscript
K.V.: Cadaver dissection, Editing manuscript, Final manuscript approval
P.G.: Cadaver dissection, Editing manuscript, Final manuscript approval
M.M.: Cadaver dissection, Editing manuscript, Final manuscript approval
W.S.: Study design, Cadaver dissection, Writing manuscript, Final manuscript approval
Disclosures
All conflicts of interest have been identified, and there has been no significant financial support or funding for this work that could have influenced its outcome.
Additional information
IRB exemption was given by Tulane University Human Research Protection Office for Study Reference#: 2021-031.

_and_lateral_(b)_imaging_confirming_correct_entry_point_pr.png)
_and_lateral_(b)_imaging_confirming_correct_entry_point_pr.png)