Introduction
Isolated ankle syndesmosis injuries account for 12% of all ankle sprains in young athletes and are more common in athletes playing certain sports including basketball.1,2 The syndesmosis is formed by 4 ligamentous structures: the anterior inferior tibiofibular ligament (AITFL), the interosseous ligament, and the posterior inferior tibiofibular ligament, and the inferior transverse ligament. The syndesmotic ligaments stabilize and facilitate the dynamic association between the tibia and fibula.3,4
Syndesmosis injury may be suspected with the mechanism of injury, with pain that is typically diffuse about the ankle or anterolaterally proximal to the ankle joint. Pain may also be associated with walking up hills, pivoting, or doing single-leg heel raises.5 The radiographic findings that indicate syndesmosis injury are increased tibiofibular clear space, Decreased tibiofibular overlap and increased medial clear space. The views demonstrating these findings are weight-bearing anteroposterior and mortise radiographs.6 However, the absence of diastasis between the distal fibula and tibia does not allow the exclusion of a syndesmotic instability.7 Magnetic resonance imaging (MRI) has been shown to have a sensitivity of 100% if performed within 6 weeks of the injury.8 An examination under anesthesia should be performed when there is a high index of suspicion without conclusive plain radiographic or MRI findings.5,9 This allows a dynamic assessment of stability for prompt diagnosis and surgical stabilization. We present a rare case of a bilateral syndesmotic injury sustained during a basketball game.
Case presentation
A 15-year-old male attended the emergency department following a basketball injury which involved a mid-air collision with another player, with bilateral ankle inversion injuries upon landing. The patient was otherwise fit and well with no other significant past medical history. As an avid basketball player, he had sustained 2 previous episodes of right ankle sprain in the previous 12 months. For both of these episodes he attended the emergency department with unremarkable and stable weightbearing ankle radiographs. He was treated with a standard RICE protocol (rest, ice, compression and elevation). He was able to return to full competition level basketball with no residual disability within 6 weeks of the episodes.
On the latest presentation, there were no open wounds or neurovascular compromise. There was a significant ankle joint effusion with tenderness of both lateral and medial malleoli of both ankles. The patient was able to weight-bear independently, despite significant pain. On plain radiograph no fracture was noted. The mortise view of both ankles revealed loss of tibiofibular overlap. With the provisional diagnosis of bilateral acute syndesmosis injury, the patient underwent an examination under anaesthesia (EUA) of both ankles.
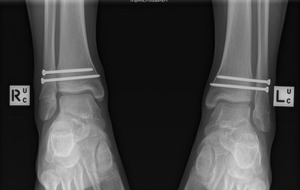
Both ankles demonstrated widening of the syndesmosis intervals when Cotton stress test was applied (Figure 1 and 2). The ankles were reduced under image intensifier and each ankle had definitive percutaneous fixation using two 3.5mm cortical screws (Synthes). Postoperatively, the patient remained non-weightbearing for 6 weeks. He was allowed to weight-bear as tolerated after 6 weeks in bilateral CAM boots and commenced gentle range of motion exercises with a physiotherapist. Radiographs at 3-months indicated enlocated and stable ankle joints with no failure of syndesmotic fixation (Figure 3). The patient underwent hardware removal and further external rotation stress tests at 3 months. There was no widening of either syndesmosis intervals. The patient progressed well with physiotherapy and was able to return to competitive basketball within 4 weeks of hardware removal. At 16 weeks after the index injury, the patient was able to achieve 30-degree flexion and 45-degree extension of both ankles and VAS pain score was 0 for both ankles at time of follow-up.
Management and outcomes
Isolated syndesmosis injuries, or high ankle sprains, may go unrecognised on initial presentation. There is often an initial misdiagnosis of a low ankle sprains that is treated non-operatively, which can lead to a delay in definitive treatment. When missed, repeated episodes of ankle instability may predispose to early degenerative changes in the ankle joint.10
Various methods can be deployed to treat acute syndesmosis injury. Screw fixation remains a commonly used approach and has demonstrated good clinical outcome with recovery, though removal of hardware after healing does contribute to additional surgery for patient.11 In comparison, fixation with tightrope has resulted in higher patient reported outcome scores, faster return to work and less surgical complications.12,13 Tightrope fixation has further contributed to economic benefit with significant cost reduction in comparison to screw fixation and its subsequent removal procedure.14
Clinical evaluation and imaging techniques have improved; however, a high index of clinical suspicion is required in order to avoid missed diagnosis. The external rotation test and squeeze test are two of the most commonly used examination for clinical diagnosis, but sensitivity remains low after correlation with MRI findings (20% and 30% respectively).15 The reliance of radiograph views such as the tibiofibular overlap in anteroposterior and mortise review is problematic as a cadaveric study has indicated no optimal radiographic parameter in assessing the syndesmotic integrity.16 Intraoperative assessment is another diagnostic method for syndesmosis injury. Whilst interobserver agreement for intraoperative assessment such as the hook test and external rotation stress test are high, the sensitivity of both tests is insufficient to determine instability of the syndesmosis intraoperatively (0.25 for hook test and 0.58 for external rotation stress test).17 Further studies have been examining arthroscopic assessment in its reliability measuring syndesmotic stability18,19 and its potential for being a future standard for diagnosis.
Vancolen et al.20 has indicated that with prompt treatment there is a high rate of return to any as well as preinjury level of sport, with mean duration being 46.4 days. The patient in this case was able to return to competitive level basketball at 16 weeks without issue. This is longer than other studies have suggested.20 The increase in duration can be attributed to the bilateral nature of the injuries, thus prolonging the rehabilitation process.
Conclusions
Isolated ankle syndesmosis injuries can occur in high ankle sprains, in particular with young athletes. Often such injuries are misdiagnosed due to lack of clinical suspicion and simple diagnostic tools to identify them. The consequence of delayed diagnosis and treatment can lead of chronic instability of the ankle joint and loss of function.21 This case report presents a rare case of acute bilateral syndesmosis injury of an active 15-year-old male who was correctly diagnosed and underwent surgical treatment in a timely fashion and is able to achieve pre-injury level of function after rehabilitation.
Authors’ contributions
LK, Orthopaedic Registrar, literature review and composition of the manuscript.
EH, Junior Medical Officer, literature review and composition of the manuscript.
MB, Consultant Orthopaedic Surgeon, treating surgeon, and composition of the manuscript.
Disclosures
There are no conflicts of interest to declare.
Further information
None of the authors are in receipt of scholarships or external funding.

_during_external_rotation_stress_test._there_is_los.png)
_during_external_rotation_stress_test._there_is_loss.png)
_during_external_rotation_stress_test._there_is_los.png)
_during_external_rotation_stress_test._there_is_loss.png)
