BACKGROUND
Unstable ankle fractures are extremely common, particularly in the elderly, even if not solely related to osteoporosis: their incidence is about 175 cases/100,000 population/year.1 Management of these injuries is still challenging because of a fairly high risk of complications.
Ankle fracture is defined as «unstable» when the integrity or stability are compromised: it occurs in case of disruption of the restraining structures on the medial side (deltoid ligament - medial malleolus), lateral side (lateral ligaments - fibular malleolus), distal tibiofibular syndesmosis and/or posterior malleolus (PM). These unstable injuries often require open reduction and internal fixation (ORIF) and because of inadequate treatment may result in permanent disability. ORIF has been demonstrated to be superior to conservative treatment: good short- or long-term results are reported, with several advantages including easier rehabilitation, early mobilization, and earlier weight-bearing. Also, stiffness and post-traumatic osteoarthritis are reduced.2
The possibility to compare functional outcomes is crucial: for this reason, patient-reported scores and questionnaires were developed. These scores assess clinical signs (pain, stiffness, swelling, etc.), function (stair-climbing, jumping, running, squatting, etc.), and daily life activities (work, sports, etc.). For ankle fractures undergoing surgical treatment, many valid and reliable scores are available.3–10 Despite that, there is truly little research published on the outcomes of their management.
The aims of this systematic review of the literature were to address four crucial questions about unstable ankle fractures: (1) What are the outcomes in the treatment of unstable ankle fractures? (2) What are the usual complications of treatment in unstable fractures? (3) What factors meanly impact the outcomes of treatment? (4) Is the fixation of the posterior malleolus crucial to restoring stability?
METHODS
Search Strategy and Criteria
For this systematic review the electronic databases PubMed, Scopus, and Embase were searched using the terms: “trimalleolar” or “bimalleolar” and “fracture” (Table 1). Articles were reviewed according to the Preferred Reported Items for Systematic Reviews and Meta-Analyses Statement for Individual Patient Data (PRISMA-IPD).11
The research questions, inclusion, and exclusion criteria were decided a priori. The inclusion criteria were:
-
human studies published in English
-
treatment of bimalleolar/trimalleolar fractures in adulthood
-
outcomes reported with scoring systems accepted in the literature
-
precisely defined follow-up
Only studies with outcomes scores were deliberately included to better compare results and to avoid vague or casual data.
Exclusion criteria were fractures in children, fractures involving joints other than the ankle (tibial pilon, Lisfranc, calcaneus…), previous arthroscopy of the ankle, isolated repair of the deltoid ligament, as well as case reports and reviews, studies on animals/cadavers, epidemiologic studies, surgical technique notes, or conservative only treatment descriptions.
Study Screening
After excluding the duplicates, two reviewers (LM, and LCZ) screened the title, abstract, and full text of each study. Disagreements were solved by discussion after a full text evaluation. The reference lists of the studies were manually searched for other publications that may have eluded the initial search.
Search Results
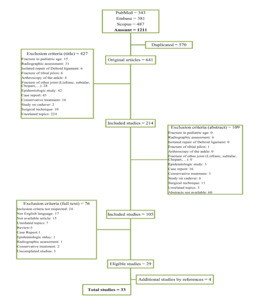
A total of 1211 articles were retrieved for preliminary evaluation (Figure 1). After the duplicates were eliminated, 641 original articles remained. Two authors (LM, LCZ) reviewed the titles: 427 studies were excluded because they did not meet the inclusion criteria. After the abstracts were reviewed, 109 studies were excluded for the same reason. Of the remaining 105 articles, 76 were excluded after evaluation of the full text. Four articles were added to 29 eligible studies from their references, for a definitive total of 33 studies enrolled in the final analysis and qualitative assessment (Table 2). All 33 studies reported data on the treatment of bimalleolar/trimalleolar fractures in adult (first and second research questions); 17 reported data on factors influencing the outcomes (third research question); 15 reported data on the role of the PM (fourth research question).
Assessment of Study Quality
Three authors (LM, LCZ, GR) independently evaluated each study for quality. For this systematic review, the Methodological Index for Non-randomized Studies (MINORS) questionnaire was used.12 The final analysis included retrospective case series (n=14), retrospective case-control studies (n=13) and prospective studies (n=6) (Table 2). The mean MINORS score for retrospective case series was 11/16 (range, 5-16); the MINORS score for the case-control studies was 16/24 (range, 12-21), and the MINORS score for randomized prospective studies was 18/24 (range, 11-23). The presence and inclusion of only six prospective studies was the main quality deficiency of the present study.
Data Collection
Data from each included study were collected, particularly the number of patients, gender, age, follow-up, outcomes, and complications (Table 3).
Functional scores, influencing co-factors, and issues about the PM obtained from the different studies were analyzed and compared. Complications associated with treatment were assessed and the frequency was reported.
RESULTS
Outcomes of ankle fractures
Concerning validated functional scores, OMAS score (n=13) and ankle-hindfoot AOFAS score (n=21) were the more frequently used. VAS scale was reported in five studies, SMFA in two studies, while AFSS score, Baird–Jackson score, and Phillips score in one study.
Olerud-Molander Ankle Score (OMAS) is a disease-specific questionnaire conceived for patients with ankle fractures and has been frequently used to evaluate subjectively scored function.3 The scale is an ordinal rating scale from 0 points (totally impaired function) to 100 points (complete function) and is based on nine different items: pain, stiffness, swelling, stair climbing, running, jumping, squatting, aids, and work/activity level. The results are divided into excellent with more than 95 points representing the best possible outcome, good with 90 to 95 points, fair with 80 to 89 points, and unsatisfactory with less than 80 points.
Excellent or good only outcomes were reported by Gupta (50% excellent, 50% good), Vem (60% excellent, 26.6% good), Choi (24% excellent, 48% good), Kukk (mean 86.0 points), Mingo (excellent or good 53.85%), Gehr (58.6% excellent, 33.3% good), Simanski (mean 90.0 points).16,19,24,29,30,33,34 Fair outcomes were reported by Testa (mean 75.3), Hong (mean 78.3),and Gehr (5.5% of cases).14,26,33 Conservative and surgical treatments were compared by means of the OMAS scale in some studies.13,17,42 Surgery tended to achieve better results: Roberts reported an OMAS score of 71.2 after fixation versus 57.3 after conservative treatment; Carter 85 points after fixation and 80 points after cast; Hoelsbrekken 81 points after surgery, 80 points after conservative treatment.13,17,42
Testa compared OMAS score based on the pattern of fracture, reporting a mean of 78.65 points in Danis-Weber Type B fractures and a mean of 69.72 points in type C fractures.14 Tanoglu compared OMAS scores after one-stage surgery (87.8 points) and after two-stage surgery (83.2) in complex fractures.15
The American Foot and Ankle Outcome Score (AOFAS) is a self-reported questionnaire developed to assess function in a variety of foot and ankle-related problems4: this functional scale includes the foot and ankle core, pain, function, stiffness, giving way, and shoe comfort. The outcome is calculated as a score of 0 to 100, with 100 representing the best possible outcome. The AOFAS score can be measured in 4 categories: excellent more than 92, good 87 to 91, fair 65 to 86, and badly less than 65.29
Most of studies reported excellent (n=6/21; range, 92.4 to 100) mean AOFAS outcomes.20,21,29,31,32,39 Mean good scores were registered by several authors (n=5; range, 87 to 91.7).22,24,25,44 Wang reported a mean fair outcome (85.7) while Jones described unsatisfactory results (59.0).28,41 Conservative and surgical treatments have been compared by two studies: even if Hoelsbrekken substantially reported similar scores (surgery 88 points, conservative 87 points), Tosun described better outcomes after fixation (92 vs 80).38,42 Tanoglu compared AOFAS scored after one-stage surgery (88.6 points) and after two-stage surgery (84.6) in complex fractures.15 Noh and Bucholz assessed patients by AOFAS score comparing metallic and biodegradable implants: the formers had better significant outcomes in both studies (respectively, 87.5 vs 84.3 and 83.0 vs 79; p<0.05).27,36
Concerning the PM, Evers reported similar AOFAS scores in large (<25%) or small (>25%) fragments (74.7 vs 75.4 points), and Kalem described better results after fixation with posterior plate (94.7 points) than with PA screw (93.4 points) or with AP screw (86.4^) [39,40]^. The posteromedial or posterolateral approach did not show any significant influence (PM 92.9, PL 91.9).40
The VAS (Visual Analogue Scale) is a generic patient-reported scale and is traditionally used only to assess the patient’s perception of pain: 0 means asymptomatic condition and 10 intolerable pain.6 Different studies indicated low scores (0-3).14,20,25,26 Testa reported better VAS scores after fixation of Weber type-B fractures (VAS 1.7) than type-C fractures (VAS 3.1).14 De Vries described similar outcomes after fixation (VAS 2.4) or conservative treatment (VAS 2.6).7 Kalem reported no differences between fixation with AP screw (VAS 0.55), PA screw (VAS 0.76), or plate (VAS 0.94).37
The Short Musculoskeletal Function Assessment (SMFA) questionnaire consists of the dysfunction index (thirty-four items assessing the patients’ function), and the bother index (twelve items evaluating how much patients are bothered by functional problems): higher scores indicate poorer function.5 O’Connor reported significant differences in outcomes comparing fixation with AP screw (20.2) and posterolateral plate (9.4).45 Noh compared metallic and biodegradable implants: at one-year follow-up, describing better outcomes with metallic implants in both indices (dysfunction: metallic 8.7 points vs biodegradable 10.5 points, p=0.060; bother: metallic 3.3 points vs biodegradable 4.6 points p=0.05).27
Baird and Jackson introduced another score based on several criteria: pain, stability of the ankle, ability to walk, run and do work, ankle movements, and radiological analysis. Scores are divided into excellent (96 to 100 points), good (91 to 95 points), fair (81 to 90 points,) and poor (80 or fewer points).8 Xing reported a mean Baird-Jackson score of 96.2 points; twenty-two cases were excellent, six cases were good, and two cases were fair. Excellent and good results were 93.3%.18
In 1985 Phillips proposed a 115-points system to document subjective and functional outcomes, including arthritis grading.9 In this system, overall scores from 110 to 115 were classified as excellent, 96 to 109 as good, 70 to 95 as fair, and less than 70 as poor.
Concerning unstable fractures of the ankle, Day described excellent or good outcomes in 64% of cases and fair or unsatisfactory in 36%.43
De Vries and Cohen evaluated the treatment of ankle fractures with the AFSS score.7,10 outcomes resulted better after surgical fixation than conservative treatment (126 vs 119).
Complications in unstable ankle fractures
Several complications were reported by the selected studies. Post-traumatic osteoarthritis was described in 7.6% to 44% after unstable ankle fractures.7,21,22,25,45 The risk of post-traumatic osteoarthritis depends on the size of fragments (small 16%, medium 48%, large 54%; p=0.006).7 Osteoarthritis occurred more frequently when there was a postoperative step-off ≥1mm on the cartilaginous surface.25 O’Connor reported wider osteoarthritis after fixation with a post-operative plate than AP screw (37.5% vs 20%).45 Regier found osteochondral lesions in 40.4% of the patients. Patients with a trimalleolar fracture had a significantly higher risk of developing an OCL compared to those with a type B fracture. The risk of developing an osteochondral lesion increased up to 5.6% when the AOFAS score decreased by one point (p=0.01).22
Wound infections were pretty common. Superficial infections were reported in 1.44 to 15.56% of patients.15,19,20,24,29,31,32,37,39,40,44 Deep infections were described in 1.9 to 13% of population.19,21,44 Wound dehiscence was in 1.8 to 2% of cases30,44 while wound reactions to implant in 5.0 to 7.2%.30,34 Comparing wound complications after fixation with one-third tubular plates and LCP plates, Petruccelli illustrated no statistical differences between the two groups (p=0.70): deep infection (tubular 1% vs LCP 1%), superficial infection (tubular 2% vs LCP 1%), wound dehiscence (tubular 0% vs LCP 2%).44
Delayed union was reported in 0 to 15% of patients.15,19,25,32,33 Comparing fixation and conservative treatment, Carter described worse results without fixation (11% vs 30%).17 Delayed union after conservative treatment was reported in 10.0% of patients by Hoelsbrekken.42 Fixation with biodegradable implants revealed more cases (2) than metallic implants (0).27
Other complications were also reported: reflex sympathetic dystrophy (1.5 to 15%),15,29,34,37 deep vein thrombosis and pulmonary embolism (0.34 to 6%),30 sural nerve injury (1.1 to 4%),21,24,36 fracture displacement (0.05-8.0%),33,40 failure of biodegradable screw (0.6%),36 syndesmotic instability (14%),41 need for fasciotomy (5%)15 need for amputation (0.16%) and mortality (1.07%).31
Failure of implant necessitating revision was described in 0.82 to 10% of cases.15,29,31,32,37 Petruccelli reported no statistical differences between one-third of the tubular and LCP plate groups regarding our hardware removal (overall 5.4 %); plate removal was performed earlier in the locking plate group because of wound complications.44
Factors influencing outcomes
Different studies aimed to assess factors that may influence the outcomes after fixation of ankle fractures. Some factors were identified by Testa and Simanski: worse outcomes were found in patients aged over 61 years, with BMI over 40, with ASA class higher than 1, affected by dementia, in type C Weber fractures or fracture-dislocations.14,34 Tanoglu reported a significant difference in outcomes between males and females: women revealed better outcomes (p=0.005), probably because ankle fractures may occur more commonly in women after low-energy trauma,15 Contrarily, Hong reported worse outcomes in females: this could be due to underlying osteopenia or osteoporosis.26
Tanoglu and Tewjani stated no significant correlation between functional scores and diabetes mellitus, hypertension, or abuse of alcohol.15,32 The involvement of tobacco addiction was contradictory: Tanoglu did not find any significant correlation, while Tewjani reported worse functional results in smokers.15,32 Poor outcomes were also found also in people with lower levels of education.32 The complexity of the fracture pattern could have also influenced the outcomes: poor long-term results were correlated to trimalleolar fractures, as the fracture of medial malleolus has been shown to be predictive of worse results.13,32 Poor AOFAS or OMAS scores were reported in patients with severe soft tissue injuries that delayed surgical treatment and increased postoperative complications.39
The correlation between outcomes and conservative rather than surgical treatments was analyzed by several authors, demonstrating worse outcomes after conservative management.13,26,32 Roberts analyzed correlations between the adequacy of reduction/fixation and the functional outcomes, identifying three key points: firstly, complex ankle fractures were more likely to be malreduced; secondly, fractures involving the PM had significantly worse outcomes, even after good reduction; lastly, the worse the malreduction the lower the functional score (OMAS score) achieved by the patient. Thus, Roberts recommended that ankle fractures should be treated only by skilled surgeons.13 The same results were found by Tewjani.32 Petruccelli assessed outcomes comparing fixation with LCP and conventional one-third tubular plate: no significant differences in radiographic bone union, time of fracture healing, or wound complication rate were found.44
Some studies assessed the correlation between functional scores and immobilization. The shorter immobilization, the better the outcomes: early rehabilitation significantly improves activity limitation and ankle range of motion, and reduces postoperative pain.19,26 These results were demonstrated in a prospective study by Simanski: early rehabilitation combined with weight-bearing was substantial in reducing the duration of the hospital stay and the return-to-work time.42
Role of the posterior malleolus (PM)
Successful functional and radiological outcomes were clearly demonstrated to be related to the fixation of the posterior malleolar fractures.7,14,16,21,38,40,45 The target of osteosynthesis is twofold: first, eliminating the eventual instability generated by the displacement of the PM; second, achieving an anatomical reduction of the articular surface in order to minimize posttraumatic osteoarthritis.14,21,37,45 Operative treatment improved functional outcomes: Tosun demonstrated lower AOFAS scores after conservative treatment compared to surgery (AOFAS 70 vs 92, p<0.001).38 Moreover, dorsiflexion was found to be significantly increased after fixation of the PM: the synthesis restored appropriate tension and integrity of the posteroinferior tibiofibular ligament.20 DeVries reported no significant difference in 13yrs-term outcomes between conservative and surgical groups. Nonetheless, the author concluded that ORIF was essential because unstable and unreduced frafracture-dislocations worse long-term outcomes.7
A matter of debate is still represented by the size of the fragment to treat: most studies recommended internal fixation for posterior malleolar fractures affecting 25% to 33% of the articular surface measured on the plain radiographs or CT. The rationale is that larger fragments led to worse long-term results than smaller fragments.16,23,24,40,45 The development of osteoarthritis occurred more frequently in fractures with medium or large-sized fragments or in the case of residual postoperative articular step-off of 1 mm or more.7,23,25,37,45 Mingo performed a statistical analysis on small (<25%) and large (>25%) fragments: the relative risks at 95%-confidence intervals revealed better AOFAS and OMAS scores in smaller fragments and demonstrated outcomes not affected by the quality of reduction.29 Nonetheless, other studies stated that even small posterior malleolar fragments may increase the risk of osteoarthritis: thus, they recommend that all fragments must be fixed regardless of size.16,20,25,37,38 Drijfhout Van Hooff reported that AOFAS and AAOS scores were not significantly worse in the larger (>25%) fragment groups compared to the smaller fragments (<5%). Hence, the author recommends syncing theis of all the fractures.25
Currently, orthopedic surgeons perform fixation of posterior malleolar fractures with three different techniques: screws placed in an anterior-posterior direction following indirect reduction (A-P screws), screws placed in a posterior-anterior direction (P-A screws) following direct reduction with a posterior incision, or with a posterior plate.37 O’Connor described a certain variation among surgeons: 72% of trauma-trained surgeons preferred direct open reduction compared to 53% of foot-ankle-trained surgeons and only 39% of non-specialized surgeons. Despite this, only 56% of trauma-trained surgeons chose posterolateral plating.45 Indirect reduction and A-P screws restored anatomic joint congruity in only 27% of patients, while restoration occurred in 83% of cases treated by a direct posterior surgical approach.24 Indeed, fixation with A-P screws showed some disadvantages. Those were the challenge to fix smaller fragments of the PM, the difficulty to judge the quality of reduction and direction of the screws under fluoroscopy, and not always being able to achieve intrinsic stability of fixation by screws alone when the injury revealed a vertical shear component.16 Kalem observed a non-statistically worse reduction in the P-A screw group compared to the A-P screw group.37 Vidovic reported no difference in complication rate between A-P fixation and P-A fixation.39 Regarding osteosynthesis by buttress plates or P-A screws, the posterolateral or posteromedial approach played a significant role in obtaining good outcomes.16 Posterior fixation provided better anatomical reduction under direct visual control, also for small or medium-sized fragments, while interfragmentary compression and biomechanical stability are improved with a buttress plate able to resist vertical shear.24,28,39,45 However, fixation through a posterior approach could also reveal some technical challenges, related to prone or lateral positioning (and consequent difficult fixation of medial malleolus), possible danger or injury of the sural nerve, and to surgery duration, because of the lesser familiarity with this technique among the surgeons.16,45
Zhong compared results deriving from posterolateral and posteromedial approaches. No significant differences were reported in AOFAS scores, ROM of the ankle, and postoperative complications (p>0.05). Hence, the author concluded that the approaches have similar clinical and radiographic outcomes and surgeons should choose the appropriate approach based on their experience.40 The posterolateral approach is not preferable in the case of simultaneous fixation of the fibula and medial malleolus: the prone position and the lateral approach can potentially lead to malreduction of the medial malleolus. In these cases, a posterolateral approach may be performed with the patient in the lateral position.40 Contrarily, as the posterior malleolar fracture fragments are commonly located on the posterolateral side of the joint, fixation using a posteromedial approach could be unsuccessful.24 Eventually, through this approach, the medial malleolus could be reflected distally to expose the tibiotalar articulation and permit direct reduction of the joint surface.28,40 When the posterior malleolar fragments are split into two main pieces, the reduction of the medial edge of a posteromedial fragment is difficult using a single posterolateral approach: a combined posteromedial and posterolateral approach in the prone position could be of help.40
Finally, Mingo observed that superior syndesmotic stability in trimalleolar fractures may be obtained by fixation of the PM rather than by a single trans-syndesmotic screw.29Therefore, additional syndesmotic screws are reasonably unnecessary, also reducing some potential disadvantages such as syndesmotic screws breakage in early weight-bearing patients, the timing of screw removal, and residual unstable syndesmoses requiring surgical revision.16
DISCUSSION
The treatment of unstable ankle fractures was vastly dealt with in literature, resulting in an advocated superiority of the surgical fixation over conservative treatment: good short- or long-term results were reported, with several advantages including easier rehabilitation, earlier mobilization, and precocious weight bearings.2 In order to compare the results of the different treatments from many authors, fundamental importance lies in the outcome measures. The most standardized and reliable scores and questionnaires reported are the OMAS score, the AOFAS score, VAS score, and SMFA score.3–10 As far as the outcomes of the treatment of unstable ankle fractures are concerned, most studies reported excellent or good results with these scores.14,16,18–21,24–26,29–34,39,43 Surgical fixation is mostly preferred over conservative treatment as it consistently returns better outcomes.7,13,17,26,32,38,42 Particularly, surgery allows for shorter immobilization and earlier weight-bearing leading to better functional scores and higher rates of return to normal life.19,26,34 As a result of this review, surgical treatment for all the unstable fractures is recommendable to restore the anatomy, function, and stability, and to reduce the risk of complications as post-traumatic arthritis was demonstrated to develop faster after conservative treatment.14,21,37,45
Interesting histological studies were performed by Tochigi and Quinn.46,47 The former demonstrated that post-traumatic osteoarthritis commonly occurred in multi-fragmentary fractures because of the death of chondrocytes near the fracture line.46 The cells’ disfunction propagates to the surrounding non-fracture areas within the first 48 hours, and its extent is related to the comminution degree, the overall length of the fracture lines, and to the intensity of the applied mechanical forces. Since the articular cartilage is avascular, biological activities of chondrocytes seemed not to be altered so much by the cartilaginous disruption and local blood supply interruption, as by the great traumatic stress on cartilage metabolism. Initially, cell necrosis occurs at the fracture line, followed by delayed apoptosis in non-fracture areas due to excessive acute mechanical stresses and the cytotoxic effect of biomechanical mediators (reactive oxygen species, matrix-damaging enzymes, inflammatory cells, and cytokines).46 Post-traumatic events occur mostly in the transitional zone of cartilage, while cell volumes per volume unit and cell surface areas per volume unit are both altered mostly on convex surfaces of the ankle.47
Accordingly, immediate restoration of the stability in ankle fractures is mandatory and advisable as instability itself tends to amplify post-traumatic osteoarthritis. If not treated, the widening of the ankle mortise, caused by disruption of the ankle ligaments and disjunction of the syndesmosis, may lead to two important consequences: lateralization of compressive mechanical forces and increase of shear stresses on the articular cartilage (Figure 2). This means that the aforementioned processes (cell apoptosis, cartilage degeneration, matrix damage) develop not only nearby the fracture lines but also in areas not directly involved by trauma. Therefore, it is clear how instability devastates the joint cartilage and why we may want to consider a “first 48hrs golden time” to limit its disruption. Performing early surgery to restore joint stability should be also more effective in inhibiting the progression of chondrocyte damage, potentially moderating the pathological cascade to post-traumatic osteoarthritis.
Surgeons should assess the pattern of fracture’s complexity as the comorbidities of the patients: the outcomes are worse in the more complicated ones (Danis-Weber Type C, fracture-dislocation, soft tissue injury) even if surgical fixation is performed lege artis.14,15,23,37 Worse outcomes have been found in older, fatter patients, with class higher operative risk, especially if affected also by dementia.14,34 Thus, the importance to inform the patient preoperatively about his condition and the really achievable results is crucial. Also, to avoid false illusions concerning outcomes, the patient should be given the information that post-traumatic osteoarthritis is the most frequent complication, correlating more to the complexity of the fracture pattern (trimalleolar, large-sized posterior fragment) than to the treatment itself.7,13,21,22,25,32
Moreover, according to the reviewed studies, metallic implants are more desirable to stabilize ankle fractures than biodegradable ones, because of the better results.27,36 Nonetheless, further research, especially with randomized prospective studies, is still desirable.
Concerning PM fractures, successful functional and radiological outcomes have been clearly demonstrated to be related to fixation.7,14,16,21,38,40,45 ORIF was traditionally indicated in case of fragment size greater than 25%-33% of the articular surface, measured on plain films or CT scans. However, several authors recently recommend fixation regardless of size, because the development of osteoarthritis has been demonstrated also in the presence of small-sized fragments.7,16,20,23,25,29,37,38,45 The treatment of choice, between conservative management or surgical treatment of the PM, should not be based only on the size of the fragment, but reducing the instability and of the displaced intra-articular fragments should also be addressed.14,21,37,45 Since the integrity of the PM plays a key role in the stability of the ankle joint and it is important for tibiotalar load transfer and posterior talar stability,48 Mingo stated that syndesmotic stability in unstable trimalleolar fractures could be achieved by fixation of the PM rather than by using a trans-syndesmotic screw.29 Miller and Ribeiro reported the same conclusion35,48 that the functional and radiographic outcomes are not significantly different by comparing fixation of posterior malleolus and syndesmosis stabilization with a screw. In addition, anatomic restoration of joint surfaces is not achieved only by stabilization of syndesmosis, as well as anatomic fixation of PM has been demonstrated to be superior to syndesmotic screw stabilization.48 Lastly, fixation of PM reduces some potential disadvantages such as syndesmotic screws breakage in early weight-bearing patients, need to screw removal, rand residual unstable syndesmoses requiring surgical revision.29,35 Contrarily, leaving screws in place can lead to many other problems: loosening, screw fatigue fracture, syndesmosis widening, tibiofibular synostosis, and osteolysis.35
Usually, the displacement of the posterior fragment is cranial, causing no mechanical impingement onto talar rotation during dorsal and plantar flexion (Figure 3). In the rare case of caudal displacement, surgical reduction and fixation are mandatory.
Moreover, the talar dome may be compared to a barrel vault, where the apex (A in Figure 3) is the keystone and the cartilaginous surface the extrados. The vault is contained by the tibial abutment, limited by anterior (B in Figure 3) and posterior (C in Figure 3) edges. In a standing position, the mechanical forces pass vertically through the talar apex, as simple compression. Indeed, during ankle motion and gait, the talar apex rotates posteriorly in dorsal flexion and anteriorly in plantar flexion, and forces are respectively transferred more anteriorly or posteriorly than the apex. Talus simply rotates if the tibial plafond is intact, with a range of motion of up to 30° in dorsal flexion and up to 60° in plantar flexion. Conversely, in the case of a PM involvement, the fracture of the tibial abutment allows a posterior shift of the talus during dorsal flexion and an anterior shift during plantar flexion, under the influence of the new compressive-tangential forces (Figure 3). Thus, if the fracture of the PM is not treated, roto-translation of the talus occurs during ankle motion and in every moment of gait, generating instability with following osteochondral lesions and osteoarthritis.
The size of the PM is crucial: the greater size of the fragment, the higher risk of talar posterior shift during dorsiflexion. Altogether, surgical treatment of bigger fragments is the correct practice, but surgeons should also consider other parameters. The normal tibiotalar axis passes through the center of the tibial plafond and the talar apex, in a lateral view. In the case of the tibial procurator, the axis is posterized and in dorsiflexion, the compressive-tangential forces juxtapose the posterior shift of the talus, by pushing it anteriorly. Conversely, in recurvatum, the axis is interiorized and forces generate roto-translation, increasing the posterior shift of the talus. Overall, surgeons should be considering the axis of the legs before choosing to surgically treat, and eventual causes for deformity should be investigated (rickets, neurofibromatosis, etc.).
During dorsal flexion, the talar keystone proportionally rotates in the posterior direction. Accordingly, for posterior fragments of the same size, the larger the dorsal flexion angle (Figure 3, α angle) the higher the risk that the talar apex could not be contained by the tibial abutment because of talar roto-translation, generating instability. Hence, a prior-to-fracture quantitative evaluation of the dorsal flexion should be obtained by assessing the healthy, contra-lateral ankle.
Moreover, selecting the approach and hardware for the PM should be depending on the pattern of the fracture and on the surgeon’s preference and experience. Fixation with P-A screws or posterior plates is advisable because they provide better anatomical reduction under direct control, also for small or medium-sized fragments, and implants can resist shear forces.16,24,39,42,45 On the other hand, fixation with A-P screws shows some disadvantages such as the challenge to fix small fragments of the PM, the difficulty to judge the reduction and direction of the screws under fluoroscopy, and reduced intrinsic stability of fixation.16,37 However, since no significant differences in complications were reported between A-P fixation and P-A fixation,39 the latter should be recommended only to experienced surgeons because of the difficulties associated with one or lateral positioning, demanding fixation of medial the malleolus and possible injury of the sural nerve.16,45
Conclusions
Surgical treatment of unstable ankle fractures has been demonstrated to result in better outcomes than conservative management and it is desirable that these fractures undergo surgery within the first 48hrs hours from trauma to reduce complications.
Different factors that may influence outcomes should be taken into account. Some are patient-related, like age, BMI, or associated comorbidities, while others are depending on the complexity of the fracture pattern or the presence of a fracture-dislocation. It is recommended to surgically stabilize the fractures of the PM, regardless of its size, but also consider preexisting deformities of the lower extremities and eventual abnormalities in the range of motion of the ankle.
ARTICLE HIGHLIGHTS
-
Surgical treatment is preferable for unstable ankle fractures.
-
Complications are strictly reduced if surgery is performed within 48hrs from trauma.
-
Posterior malleolus should be surgically stabilized regardless of size.
-
Preexisting deformities of the lower extremities and ankle ROM must be considered.
CONFLICT OF INTEREST STATEMENT
Each author certifies that he/she has no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
AUTHOR CONTRIBUTIONS
L Monestier, G Riva and L Coda Zabetta reviewed the literature and contributed to manuscript drafting; L Monestier and G Riva analyzed the imaging findings; MF Surace, L Monestier and G Riva were responsible for the revision of the manuscript for important intellectual content; all authors issued final approval for the version to be submitted.